Photographer Captures 'Last Stop' in Britain's Covid War
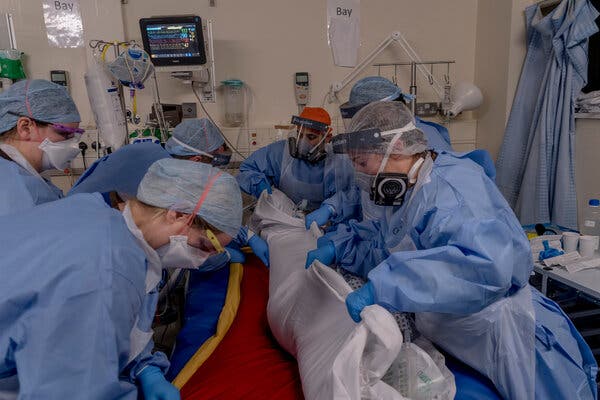
#masthead-section-label, #masthead-bar-one { display: none }The Coronavirus OutbreakliveLatest UpdatesMaps and CasesRisk Near YouVaccine RolloutNew Variants TrackerAdvertisementContinue reading the main storySupported byContinue reading the main storyTimes Insider‘This Is the Last Stop’: Shooting Britain’s Struggle Against CovidAfter receiving access to hospitals, nursing homes and burial sites, I saw up close the nation’s agony, and grit.Health care workers in the intensive care unit at the Homerton hospital in London turn a patient onto her back to help her breathe.Credit…Andrew Testa for The New York TimesMarch 2, 2021, 5:00 a.m. ETTimes Insider explains who we are and what we do, and delivers behind-the-scenes insights into how our journalism comes together.I had covered wars before, in the Balkans and Afghanistan. They were shooting wars where journalists — often foolishly — convinced themselves that they had a chance of identifying and sidestepping danger.But in Britain’s war against Covid-19, the days I spent as a freelance photojournalist covering the intensive care unit of the Homerton hospital in East London involved danger with every breath. The project for The New York Times documenting the nation’s fight against the coronavirus was terrifying and awe-inspiring. Terrifying because of potential exposure to an invisible killer that has claimed over 120,000 lives in Britain and more than 2.5 million globally. Awe-inspiring because I could witness the remarkable courage, professionalism and sheer grit of medical personnel whose daily routines placed them on the very cusp of life and death.Even the most advanced modern medicine offers no magic cures. For those who can’t make it out of the I.C.U., there is only death. This is the last stop. What stayed with me afterward was the fear in people’s eyes as they joined what could be the final battle. For the medical staff, the burden of responsibility is enormous.As Britain approaches a gradual loosening of its most draconian lockdown, and with millions of people securing access to vaccines, images of this terminal conflict do not fit easily into the official narrative.A vaccination center inside the Cathedral in Salisbury. Credit…Andrew Testa for The New York TimesMany Britons are probably unaware of the brutal reality of the I.C.U.: the constant bleeps of monitors everywhere; the staff hurrying to flip over, or “prone,” patients to help them breathe; the all-too-brief respites that give way to frenetic activity.Raising this awareness took months. My editors — Gaia Tripoli in London and David Furst in New York — and the researcher Amy Woodyatt and I called hospitals, mortuaries, crematories, funeral parlors and ambulance depots seeking access to chronicle this moment in the pandemic, only to be turned down. Often, we were told that photography was incompatible with the dignity of the dead.Finally, some were willing to cooperate, and after I was able to observe their toil, we began to assemble a portfolio to tell the story of Britain’s struggle. We wanted our images to reflect more than one area of London or one ethnic group. The list of subjects grew from a care home in Scarborough on the northeastern coast, to a funeral director in the English Midlands, to those dealing with Islamic and other rites in the capital.Prayers before a burial of a Muslim victim. One aim of the project was to avoid representing just one ethnic group in Britain that has been affected. Credit…Andrew Testa for The New York TimesWith this assignment came a new and unfamiliar set of ground rules and procedures designed to protect not only me but also those around me — both at work and at home..css-1xzcza9{list-style-type:disc;padding-inline-start:1em;}.css-c7gg1r{font-family:nyt-franklin,helvetica,arial,sans-serif;font-weight:700;font-size:0.875rem;line-height:0.875rem;margin-bottom:15px;color:#121212 !important;}@media (min-width:740px){.css-c7gg1r{font-size:0.9375rem;line-height:0.9375rem;}}.css-1sjr751{-webkit-text-decoration:none;text-decoration:none;}.css-1sjr751 a:hover{border-bottom:1px solid #dcdcdc;}.css-rqynmc{font-family:nyt-franklin,helvetica,arial,sans-serif;font-size:0.9375rem;line-height:1.25rem;color:#333;margin-bottom:0.78125rem;}@media (min-width:740px){.css-rqynmc{font-size:1.0625rem;line-height:1.5rem;margin-bottom:0.9375rem;}}.css-rqynmc strong{font-weight:600;}.css-rqynmc em{font-style:italic;}.css-yoay6m{margin:0 auto 5px;font-family:nyt-franklin,helvetica,arial,sans-serif;font-weight:700;font-size:1.125rem;line-height:1.3125rem;color:#121212;}@media (min-width:740px){.css-yoay6m{font-size:1.25rem;line-height:1.4375rem;}}.css-1dg6kl4{margin-top:5px;margin-bottom:15px;}.css-16ed7iq{width:100%;display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-align-items:center;-webkit-box-align:center;-ms-flex-align:center;align-items:center;-webkit-box-pack:center;-webkit-justify-content:center;-ms-flex-pack:center;justify-content:center;padding:10px 0;background-color:white;}.css-pmm6ed{display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-align-items:center;-webkit-box-align:center;-ms-flex-align:center;align-items:center;}.css-pmm6ed > :not(:first-child){margin-left:5px;}.css-5gimkt{font-family:nyt-franklin,helvetica,arial,sans-serif;font-size:0.8125rem;font-weight:700;-webkit-letter-spacing:0.03em;-moz-letter-spacing:0.03em;-ms-letter-spacing:0.03em;letter-spacing:0.03em;text-transform:uppercase;color:#333;}.css-5gimkt:after{content:’Collapse’;}.css-rdoyk0{-webkit-transition:all 0.5s ease;transition:all 0.5s ease;-webkit-transform:rotate(180deg);-ms-transform:rotate(180deg);transform:rotate(180deg);}.css-eb027h{max-height:5000px;-webkit-transition:max-height 0.5s ease;transition:max-height 0.5s ease;}.css-6mllg9{-webkit-transition:all 0.5s ease;transition:all 0.5s ease;position:relative;opacity:0;}.css-6mllg9:before{content:”;background-image:linear-gradient(180deg,transparent,#ffffff);background-image:-webkit-linear-gradient(270deg,rgba(255,255,255,0),#ffffff);height:80px;width:100%;position:absolute;bottom:0px;pointer-events:none;}#masthead-bar-one{display:none;}#masthead-bar-one{display:none;}.css-1pd7fgo{background-color:white;border:1px solid #e2e2e2;width:calc(100% – 40px);max-width:600px;margin:1.5rem auto 1.9rem;padding:15px;box-sizing:border-box;}@media (min-width:740px){.css-1pd7fgo{padding:20px;width:100%;}}.css-1pd7fgo:focus{outline:1px solid #e2e2e2;}#NYT_BELOW_MAIN_CONTENT_REGION .css-1pd7fgo{border:none;padding:20px 0 0;border-top:1px solid #121212;}.css-1pd7fgo[data-truncated] .css-rdoyk0{-webkit-transform:rotate(0deg);-ms-transform:rotate(0deg);transform:rotate(0deg);}.css-1pd7fgo[data-truncated] .css-eb027h{max-height:300px;overflow:hidden;-webkit-transition:none;transition:none;}.css-1pd7fgo[data-truncated] .css-5gimkt:after{content:’See more’;}.css-1pd7fgo[data-truncated] .css-6mllg9{opacity:1;}.css-k9atqk{margin:0 auto;overflow:hidden;}.css-k9atqk strong{font-weight:700;}.css-k9atqk em{font-style:italic;}.css-k9atqk a{color:#326891;-webkit-text-decoration:none;text-decoration:none;border-bottom:1px solid #ccd9e3;}.css-k9atqk a:visited{color:#333;-webkit-text-decoration:none;text-decoration:none;border-bottom:1px solid #ddd;}.css-k9atqk a:hover{border-bottom:none;}Covid-19 Vaccines ›What You Need to Know About the Vaccine RolloutProviders in the U.S. are administering about 1.3 million doses of Covid-19 vaccines per day, on average. Almost 30 million people have received at least one dose, and about 7 million have been fully vaccinated. How many people have been vaccinated in your state?The U.S. is far behind several other countries in getting its population vaccinated.In the near future, travel may require digital documentation showing that passengers have been vaccinated or tested for the coronavirus.When can you get the vaccine? What are the vaccine’s side effects? Is it safe to take during pregnancy? We’ve have answers to many of your questions. In the Homerton I.C.U., they called it “donning and doffing” of personal protective equipment. I switched my day clothes for scrubs and a surgical gown; a close-sealing mask and goggles; overshoes; and a hair covering. I pared down my equipment to two cameras. And at the end of the day’s shooting, I followed a very strict protocol developed by the I.C.U. staff for removing protective gear.Once home, I laundered all my clothes, showered, cleaned equipment with anti-viral wipes and exposed it to a UVC light sanitizer. I was not eligible to be vaccinated, but I had a precautionary coronavirus test during the assignment that came up negative.The I.C.U. in the Homerton hospital. Shooting in the unit required following a strict set of safety rules. Credit…Andrew Testa for The New York TimesUltimately, I told myself, I just had to trust my equipment. But there is always gnawing doubt. The coronavirus frightens you twice over: first by its ability to infect you personally, and second by the overwhelming fear that you might inadvertently pass it on to your family.There is never any question about its power. On my second day in the Homerton I.C.U., two people died within 25 minutes of each other. Usually, the medical authorities try to provide access for family members to say goodbye. But with patients in induced comas and beyond hope, it is a cruelly one-sided exchange of farewells.And yet the counter-imagery of dedication is always there, too, just as evident in these images as the losses. As one survivor remarked, the medical teams always go the extra mile. “They are blessed,” he said.AdvertisementContinue reading the main story
Read more →