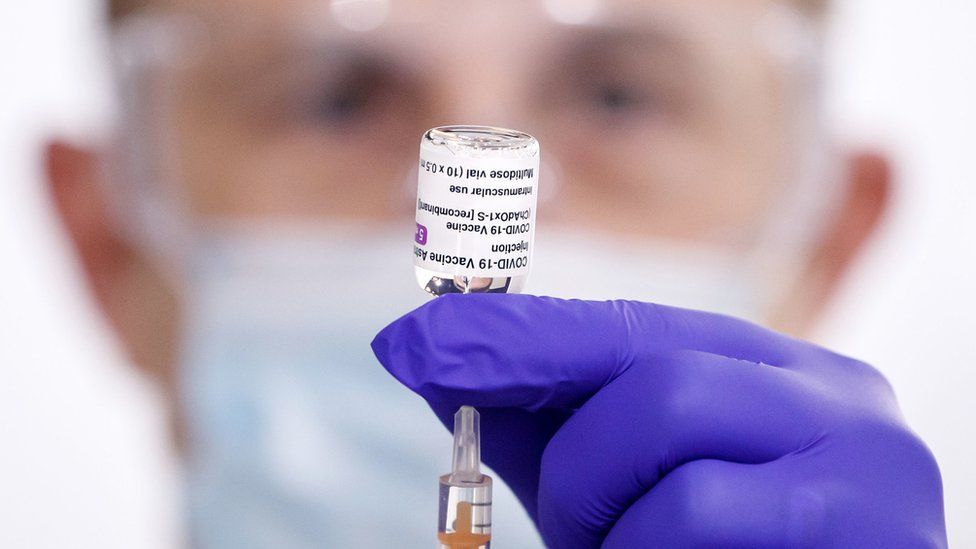
Mixing Covid vaccines gives good protection, study suggests
SharecloseShare pageCopy linkAbout sharingimage copyrightPA MediaA mix-and-match approach to Covid vaccines – using different brands of jab for first and second doses – gives good protection against the pandemic virus, a UK study has found.The Com-Cov trial looked at the efficacy of either two doses of Pfizer, two of AstraZeneca, or one of them followed by the other. All combinations worked well, priming the immune system.This knowledge could offer flexibility for vaccine rollout, say experts. The UK’s deputy chief medical officer, Prof Jonathan Van-Tam, said there was no reason to change the current successful same dose vaccine schedules in the UK, however, given vaccines were in good supply and saving lives.But he says it might be something to look at in the future: “Mixing doses could provide us with even greater flexibility for a booster programme, while also supporting countries who have further to go with their vaccine rollouts, and who may be experiencing supply difficulties.”Some countries are already using mixed doses. Spain and Germany are offering the Pfizer or Moderna mRNA vaccines as a second dose to younger people who have already received a first dose of the AstraZeneca vaccine, following concerns about rare but serious blood clots, rather than about efficacy.Rare blood clots – what you need to knowTwo doses are important to give the fullest protection and teach the body to make antibodies and T cells to block and kill Covid. The Com-Cov study, which looked at giving the doses four weeks apart in 850 volunteers aged 50 and above, found:AZ followed by Pfizer induced higher antibodies and T cell responses than Pfizer followed by AZBoth of these mixes induced higher antibodies than two doses of AZThe highest antibody response was seen after two doses of Pfizer, and the highest T cell response from AZ followed by PfizerLead investigator Prof Matthew Snape, from the University of Oxford, said the findings did not undermine the UK policy of giving people the same jab twice: “We already know that both standard schedules are very effective against severe disease and hospitalisations, including against the Delta variant when given at eight to 12 weeks apart.”He said the new results showed mixed dose schedules were also effective, even though the interval of four weeks studied was shorter than the eight to 12-week schedule most commonly used in the UK.”This longer interval is known to result in a better immune response,” he added. Mixed dose trial results for a 12-week jab interval will be available next month.Autumn booster dose?Meanwhile, another pre-print study, which also came out on Monday, suggests a third dose of AZ vaccine, given more than six months after the second, boosts the immune system.But experts say it is too early to know if people will need a booster dose this year ahead of winter. It is unclear yet how much immunity might wane over time. Prof Paul Hunter from the University of East Anglia said: “The big question at present is whether or not we will be being offered booster vaccines in the autumn. With the evidence available from this and other sources, I suspect that will be likely for those most at risk from the virus, either due to age or being clinically vulnerable.”He suggested people who have had a first course of AstraZeneca might be offered the Pfizer vaccine in as a booster rather than a repeat AstraZeneca, while people who had a Pfizer first course may not need an autumn booster, based on the evidence from the Com-Cov trial. Related Internet LinksCom-CoVThe BBC is not responsible for the content of external sites.
Read more →