Scientists discover brain layers that get stronger with age
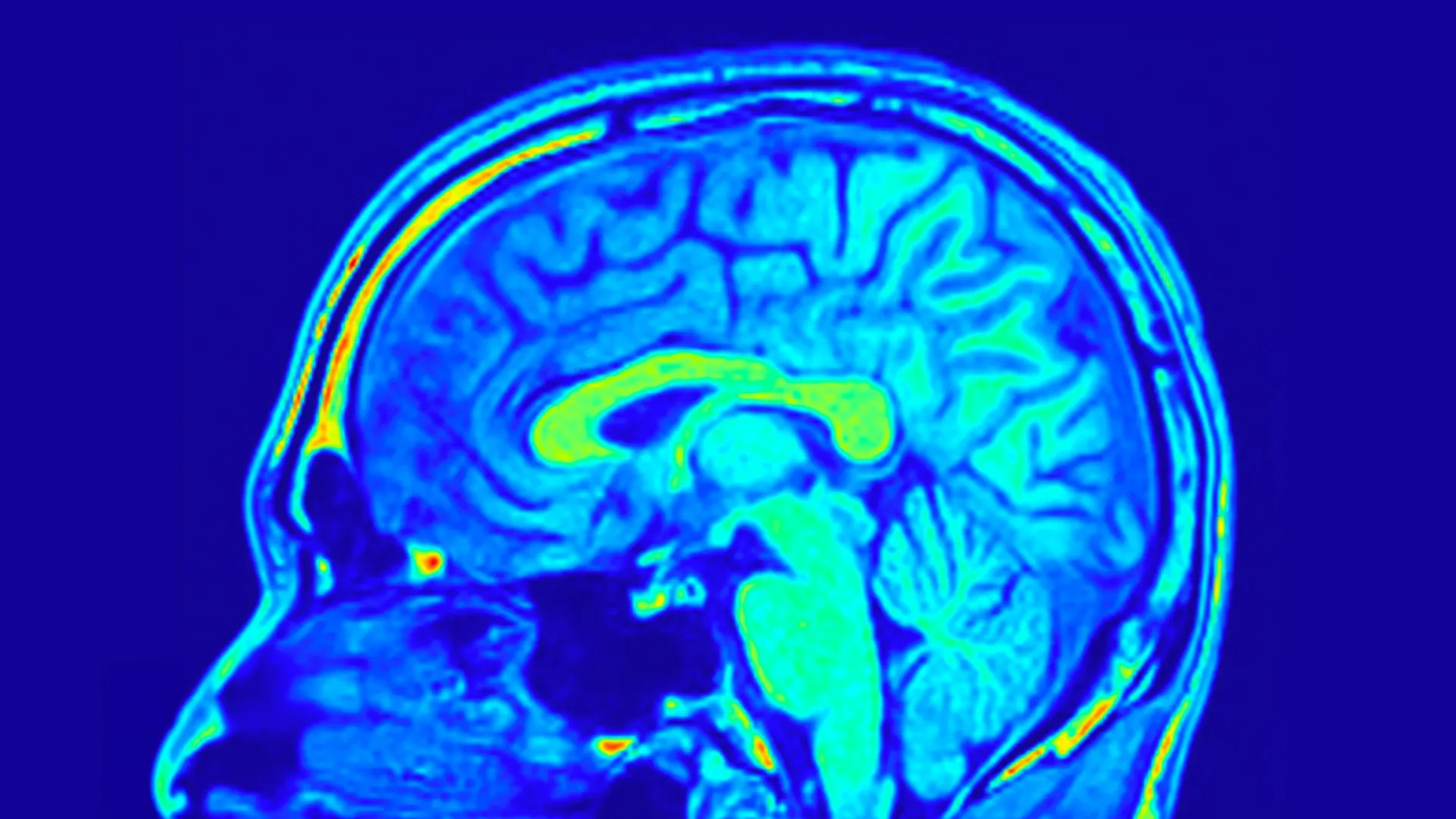
The human brain ages less than thought and in layers – at least in the area of the cerebral cortex responsible for the sense of touch. Researchers at DZNE, the University of Magdeburg, and the Hertie Institute for Clinical Brain Research at the University of Tübingen come to this conclusion based on brain scans of young and older adults in addition to studies in mice. Their findings, published in the journal Nature Neuroscience, also provide new insights into how the ability to process sensory information changes with age.
The human cerebral cortex is only a few millimeters thick and arranged in numerous folds. This tissue usually becomes thinner with age. “This is a hallmark of aging. It is attributed, among other things, to the loss of neurons. As a result, some abilities deteriorate. In any case, it is generally assumed that less brain volume means reduced function,” explains Prof. Esther Kühn, a neuroscientist at DZNE and the Hertie Institute for Clinical Brain Research. “However, little is known about how exactly the cortex actually ages. This is remarkable, given that many of our daily activities depend on a functioning cortex. That’s why we examined the situation with high-resolution brain scans.”
A processor for tactile input
Together with colleagues from Tübingen and Magdeburg, Esther Kühn focused on a part of the cerebral cortex where signals from the tactile sense are processed. This “primary somatosensory cortex” is located on the left and right side of the top of the head and extends along a strip about a finger’s width wide towards each ear. “This brain area is relevant for the perception of one’s own body and for interacting with the environment,” explains the neuroscientist. “When I pick up a key, grasp a door handle or even walk, I constantly need haptic feedback to control my movements. The corresponding stimuli converge in this area and are also processed here.”
An unexpected finding
Using magnetic resonance imaging (MRI), the researchers were able to map this area of the cerebral cortex with unprecedented accuracy. To do this, they employed a particularly sensitive scanner with a magnetic field strength of seven Tesla, enabling them to image minute brain structures about the size of a grain of sand. A total of around 60 women and men between the ages of 21 and 80 were examined. “Until now, it had not been considered that the primary somatosensory cortex consists of a stack of several extremely thin layers of tissue, each with its own architecture and function. We have now found that these layers age differently. Although the cerebral cortex becomes thinner overall, some of its layers remain stable or, surprisingly, are even thicker with age. Presumably because they are particularly solicited and thus retain their functionality. We therefore see evidence for neuroplasticity, that is, adaptability, even in senior people.”
Stacked architecture
The layered structure of the primary somatosensory cortex also occurs in similar form in other areas of the human brain – and even in other organisms. “From an evolutionary perspective, processing sensory information in this way has apparently proven beneficial,” says Kühn. In the current study, not only the middle layer of the cortex but also the areas above were found to be remarkably resistant to the aging process. The different layers were distinguished based on their content of myelin, a substance essential for the transmission of nerve signals. “The middle layer is effectively the gateway for haptic stimuli. In the layers above, further processing occurs,” says Kühn. “For example, in the case of sensory stimuli from the hand, the upper layers are particularly involved in the interaction between neighboring fingers. This is important when grasping objects. We therefore also did tests on the tactile sensitivity and motor ability of the hand with our study participants. Furthermore, we performed so-called functional MRI scans to capture the function of the middle layer of the cortex, where the signals are received.”
Modulated stimuli
Only the deeper layers of the cerebral cortex showed age-related degeneration: they were thinner in older study participants than in younger ones. In the lower layers of the cortex, a process called modulation takes place: tactile signals are amplified or attenuated depending on the context. “This has something to do with concentration and attention,” explains Kühn. “For example, if I’m wearing a ring on my finger, at some point I’ll stop feeling it, even though the tactile stimuli are still there. This only reoccurs when I consciously notice the ring again.”
What is used is preserved
“The middle and upper layers of the cortex are most directly exposed to external stimuli. They are permanently active because we have constant contact with our environment,” Kühn continues. “The neural circuits in the lower layers are stimulated to a lesser extent, especially in later life. I therefore see our findings as an indication that the brain preserves what is used intensively. That’s a feature of neuroplasticity. This is also consistent with our observations regarding a study participant, who was 52 years old. He had to rely on just one arm throughout his life, as he was born with a missing limb. The corresponding middle layer of his cerebral cortex, the one getting sensory inputs, was comparatively thin.” In addition, differences in the aging of the brain’s layers may explain why some abilities decline with age, while others do less. “Sensorimotor skills that are repeatedly practiced, such as typing on a keyboard, can remain stable for a long time, even in old age,” says Kühn. “However, if there are interfering stimuli, such as a noisy environment, older people usually find such activities particularly difficult. This could be because the functionality of the deep layers of the cortex has deteriorated, the modulation of sensory stimuli thus being impaired.”
Evidence for compensation
However, the researchers found evidence that mechanisms in the deep layers of the cerebral cortex counteract age-related functional decline to some extent. “Although the deep layers became thinner with age, their myelin content, surprisingly, increased. In fact, we also observed these effects in studies on mice, which we did for comparison. We then found that the rise in myelin is due to an increase in the number of certain neurons,” says Kühn. “These are known to have a positive effect on the modulation of nerve impulses. They sharpen the signal, so to speak. Apparently, compensatory mechanisms counteract specific cellular degeneration. With regard to prevention, it would be interesting to study whether these mechanisms can be specifically promoted and maintained. In fact, our data from mice suggests that this compensation disappears at a very advanced age.”
An optimistic view on aging
“Together, our findings are consistent with the general idea that we can do something good for our brains with appropriate stimulation. I think it’s an optimistic notion that we can influence our aging process to a certain degree,” says Kühn. “But of course, everyone has to find their own way to tap into this potential.”