People who had lost their sight have regained the ability to read after receiving an innovative electronic eye implant paired with augmented-reality glasses, according to a clinical trial involving researchers from UCL (University College London) and Moorfields Eye Hospital.
Published in The New England Journal of Medicine, the European trial reported that 84% of participants could once again recognize letters, numbers, and words using prosthetic vision in an eye that had previously gone blind due to geographic atrophy caused by dry age-related macular degeneration (AMD), a currently untreatable condition.
Participants treated with the device were able to read an average of five lines on a standard vision chart. Before surgery, several could not even distinguish the chart at all.
Breakthrough Study and Participants
The study enrolled 38 patients across 17 hospitals in five countries, testing a pioneering implant known as PRIMA. Moorfields Eye Hospital served as the only UK site. All participants had completely lost central vision in the treated eye before receiving the implant.
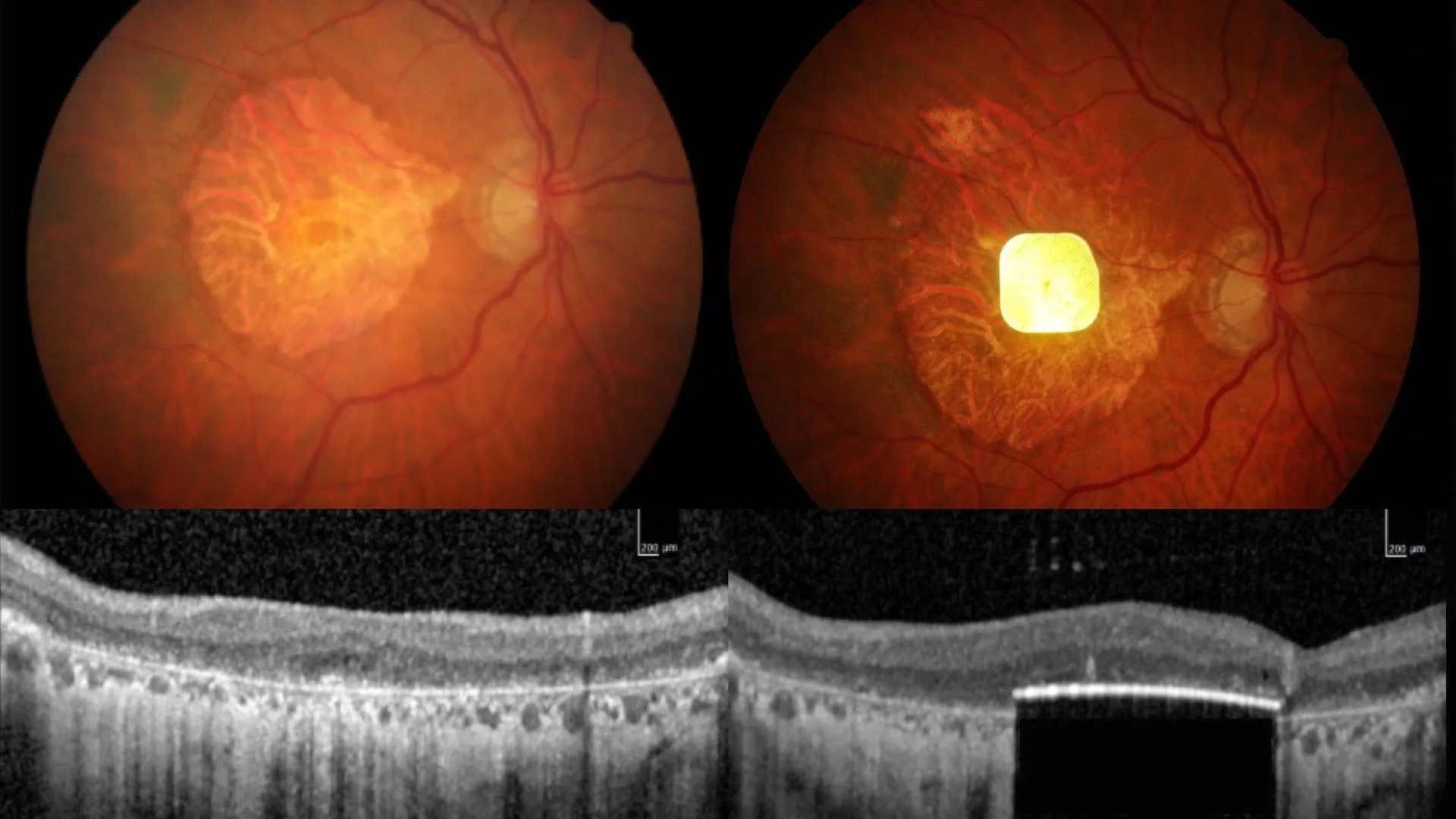
Dry AMD gradually destroys the light-sensitive cells of the macula, eroding central vision over time. In its advanced stage, called geographic atrophy (GA), the degeneration can lead to total blindness in the affected eye as the central macula deteriorates. Around 5 million people worldwide live with GA, for which no treatment currently exists. Those enrolled in the study retained only peripheral vision.
This implant is the first of its kind capable of restoring the ability to read letters, numbers, and words through an eye that had lost its sight.
A New Era of Artificial Vision
Mr. Mahi Muqit, associate professor at the UCL Institute of Ophthalmology and senior vitreoretinal consultant at Moorfields Eye Hospital, led the UK arm of the trial. He said: “In the history of artificial vision, this represents a new era. Blind patients are actually able to have meaningful central vision restoration, which has never been done before.
“Getting back the ability to read is a major improvement in their quality of life, lifts their mood and helps to restore their confidence and independence. The PRIMA chip operation can safely be performed by any trained vitreoretinal surgeon in under two hours — that is key for allowing all blind patients to have access to this new medical therapy for GA in dry AMD.”
How the PRIMA Implant Works
The procedure begins with a vitrectomy, where the eye’s vitreous gel is removed from between the lens and the retina. The surgeon then inserts a microchip shaped like a SIM card, only 2mm by 2mm, beneath the central retina through a small opening.
After surgery, patients use augmented-reality glasses equipped with a video camera linked to a pocket-sized computer with a zoom feature worn at the waist.
About a month after surgery, once the eye has healed, the implant is activated. The glasses’ camera captures visual scenes and projects them as an infra-red beam across the chip. Artificial intelligence (AI) algorithms in the computer process this data and convert it into electrical signals, which travel through retinal and optic nerve cells to the brain. The brain interprets these signals as images, allowing patients to perceive vision.
With training, patients learn to scan text using the glasses and adjust the zoom to read. Each participant underwent several months of rehabilitation to interpret these new signals and regain reading skills.
No participant experienced a decline in their remaining peripheral vision. The results pave the way for regulatory approval of the device and broader clinical use.
Patient Story: Seeing Words Again
Sheila Irvine, one of Moorfields’ patients on the trial who was diagnosed with age-related macular degeneration, said: “I wanted to take part in research to help future generations, and my optician suggested I get in touch with Moorfields. Before receiving the implant, it was like having two black discs in my eyes, with the outside distorted.
“I was an avid bookworm, and I wanted that back. I was nervous, excited, all those things. There was no pain during the operation, but you’re still aware of what’s happening. It’s a new way of looking through your eyes, and it was dead exciting when I began seeing a letter. It’s not simple, learning to read again, but the more hours I put in, the more I pick up.
“The team at Moorfields has given me challenges, like ‘Look at your prescription’, which is always tiny. I like stretching myself, trying to look at the little writing on tins, doing crosswords.
“It’s made a big difference. Reading takes you into another world, I’m definitely more optimistic now.”
The global trial was led by Dr. Frank Holz of the University of Bonn, with participants from the UK, France, Italy and the Netherlands.
The PRIMA System device used in this operation is being developed by Science Corporation (science.xyz), which develops brain-computer interfaces and neural engineering.
More About the Device
The device is a novel wireless subretinal photovoltaic implant paired with specialised glasses that project near-infrared light to the implant, which acts like a miniature solar panel.
It is 30 micrometers/microns (0.03mm) thick, about half the thickness of a human hair.
A zoom feature gives patients the ability to magnify letters. It is implanted in the subretinal layer, under the retinal cells that have died. Until the glasses and waistband computer are turned on, the implant has no visual stimulus or signal to pass through to the brain.
In addition to practicing their reading and attending regular training, patients on the trial were encouraged to explore ways of using the device. Sheila chose to learn to do puzzles and crosswords while one of the French patients used them to help navigate the Paris Metro — both tasks being more complex than reading alone.
Further quotes from Mr. Mahi Muqit, UCL and Moorfields clinical researcher:
“My feeling is that the door is open for medical devices in this area, because there is no treatment currently licensed for dry AMD — it doesn’t exist.
“I think it’s something that, in future, could be used to treat multiple eye conditions.
“The rehabilitation process is key to these devices. It’s not like you’re popping a chip in the eye and then you can see again. You need to learn to use this type of vision.
“These are elderly patients who were no longer able to read, write or recognize faces due to lost vision. They couldn’t even see the vision chart before. They’ve gone from being in darkness to being able to start using their vision again, and studies have shown that reading is one of the things patients with progressive vision loss miss most.”
Read more →