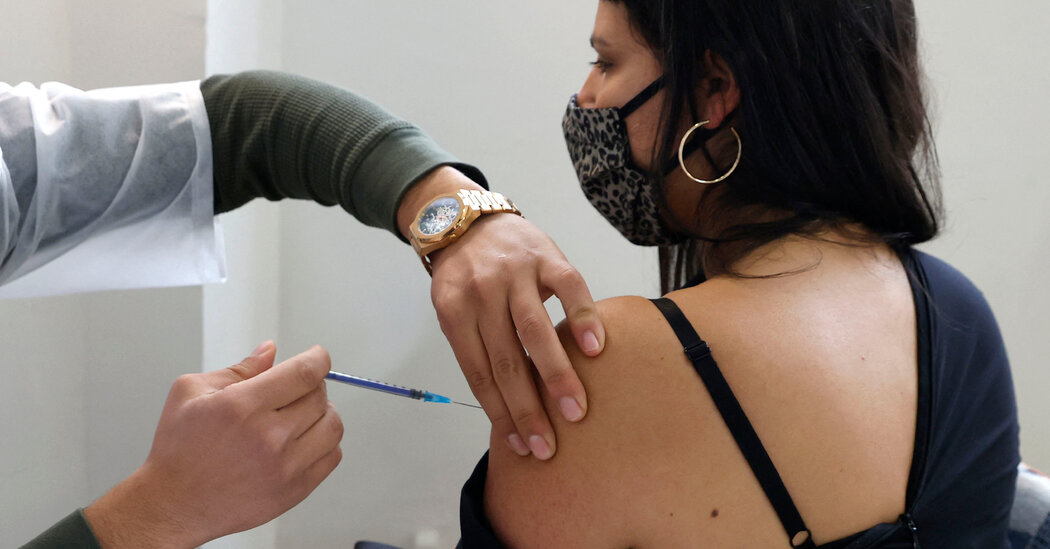
Two studies showed the vaccine to be more than 95 percent effective at protecting against severe disease or death from the variants first identified in South Africa and the U.K.The Pfizer-BioNTech coronavirus vaccine is extraordinarily effective at protecting against severe disease caused by two dangerous variants, according to two studies published Wednesday.The studies, which are based on the real-world use of the vaccine in Qatar and Israel, suggest that the vaccine can prevent the worst outcomes — including severe pneumonia and death — caused by B.1.1.7, the variant first identified in the U.K., and B.1.351, the variant first identified in South Africa.“This is really good news,” said Dr. Annelies Wilder-Smith, an infectious disease researcher at the London School of Hygiene and Tropical Medicine. “At this point in time we can confidently say that we can use this vaccine, even in the presence of circulating variants of concern.”Previous research suggested that B.1.1.7 is more infectious and more deadly than other variants, but that vaccines still worked well against it. But vaccines appeared to be less effective against B.1.351, according to earlier studies.One of the new studies, which appeared in the New England Journal of Medicine, is based on information about more than 200,000 people that was pulled from Qatar’s national Covid-19 databases between Feb. 1 and March 31.During that time, the variants were widespread there: Sequencing conducted between Feb. 23 and March 18 suggested that roughly half of the coronavirus infections in that period were caused by B.1.351 and 44.5 percent were caused by B.1.1.7.In multiple analyses, the researchers found that the vaccine was 87 to 89.5 percent effective at preventing infection with B.1.1.7 among people who were at least two weeks past their second shot. It was 72.1 to 75 percent effective at preventing infection with B.1.351 among those who had reached the two-week point.Even that slightly reduced effectiveness against infection with B.1.351 is still largely good news, one of the study’s authors, Laith Abu-Raddad, an infectious disease epidemiologist at Weill Cornell Medicine-Qatar, said. “We’re talking about a variant which is probably the nastiest of all the variants of concern,” he said. “It’s not the 95 percent we were hoping, but the 75 percent is really great.”The vaccine was highly effective at protecting against the worst outcomes. Over all, it was 97.4 percent effective at preventing severe, critical or fatal disease from any form of the coronavirus, and 100 percent effective at preventing severe, critical or fatal disease caused by B.1.1.7 or B.1.351. (This slight difference in effectiveness is likely a result of the fact that the sample sizes were smaller for the subgroups of patients with a documented variant, Dr. Abu-Raddad said.)The second new study, which was published in The Lancet, was conducted by researchers at the Israel Ministry of Health and Pfizer. It is based on more than 230,000 coronavirus infections that occurred in Israel between Jan. 24 and April 3. During that period, B.1.1.7 accounted for nearly 95 percent of all coronavirus cases in the country, which has vaccinated more than half of its population.The researchers found that the vaccine was more than 95 percent effective at protecting against coronavirus infection, hospitalization and death among fully vaccinated people 16 and older. It also worked well in older adults. Among those 85 or older, the vaccine was more than 94 percent effective at protecting against infection, hospitalization and death.As the percentage of fully vaccinated people in each age group grew, the incidence of coronavirus infections in that cohort fell, the researchers found. The declines in infection rates matched the timing of increasing vaccine coverage in each age group better than the start of a nationwide lockdown. The results suggest that Israel’s rapid pace of vaccination has been responsible for the decline in infections in the country.“I’m just really happy to see this data that in the real world these vaccines are having such an amazing impact on curtailing infection and disease,” said Akiko Iwasaki, an immunologist at Yale University.Both studies also reported that two doses of the vaccine provided significantly more protection than one dose did. In the Israel study, for example, one dose of the vaccine was 77 percent effective against death, while two doses were 96.7 percent effective.“It absolutely emphasizes the need for the second dose,” said Dr. Kathleen Neuzil, who directs the Center for Vaccine Development and Global Health at the University of Maryland School of Medicine.Together, the studies suggest that even with the new variants, vaccination remains a plausible path out of the pandemic, experts said. “If we can get vaccines to the world and get coverage up,” Dr. Neuzil said, “I believe we can get on top of this and we can get on top of the emergence of new variants.”
Read more →