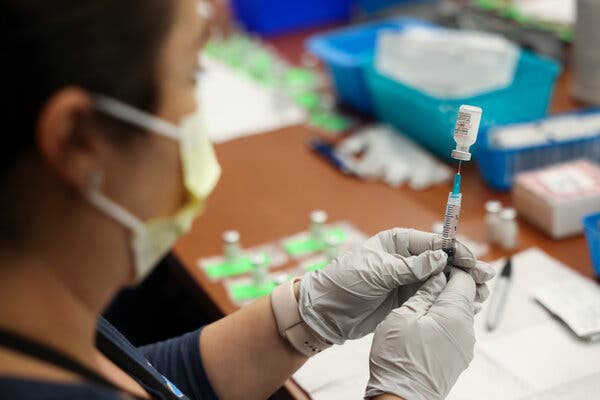
The F.D.A.’s authorization of Pfizer’s Covid shot for 12- to 15-year-olds is a milestone in battling the coronavirus, but actually getting them vaccinated involves new challenges.Abby Goodnough and Hundreds of high school seniors rode in bus caravans recently to a mass vaccination site outside Hartford, Conn., where they got Covid-19 shots as a D.J. played Lady Gaga and a selfie backdrop awaited.Now, the race is on to get to their younger siblings — and all the nation’s nearly 17 million 12- to 15-year-olds, after the Food and Drug Administration authorized the Pfizer-BioNTech vaccine for their age group.The F.D.A.’s decision, announced Monday afternoon, presents a bright new opportunity in the push for broad immunity against the coronavirus in the United States, but the challenges are more daunting than for immunizing older, more independent teenagers.A recent survey by the Kaiser Family Foundation’s Vaccine Monitor found that many parents — even those who eagerly got their own Covid shots — are reluctant to vaccinate pubescent children. Yet doing so will be critical for further reducing transmission of the virus, smoothly reopening middle and high schools and regaining some sense of national normalcy.“The game changes when you go down as young as 12 years old,” said Nathan Quesnel, the superintendent of schools in East Hartford, adding, “You need to have a different level of sensitivity.”States, counties and school districts around the country are trying to figure out the most reassuring and expedient ways to reach younger adolescents as well as their parents, whose consent is usually required by state law. They are making plans to offer vaccines not only in schools, but also at pediatricians’ offices, day camps, parks and even beaches.Children’s Minnesota, a Minneapolis-based hospital system where the main Covid vaccination site has offered stress balls, colored lights and images of playful dolphins projected on the ceiling, is planning to provide shots beginning later this week in at least a dozen middle schools and a Y.W.C.A.In Columbus, Ohio, public health nurses will drive a mobile vaccination unit around neighborhoods “just like you would an ice cream truck,” said Dr. Mysheika Roberts, the city health commissioner. In Connecticut, Community Health Center, a statewide primary care provider that vaccinated the busloads of high school seniors, is aiming to reach younger adolescents by offering shots at amusement parks, beaches and camps, among other locales.“You’re going to Dollar General?” said Yvette Highsmith-Francis, a vice president of Community Health Center. “Guess what? We’re in the parking lot.”But with the school year ending soon, many health officials are racing against the academic clock to schedule both recommended doses, seeing schools as the best place to reach many students at once.A vial of the Pfizer vaccine at the Denver School of Science and Technology Green Valley Ranch this month.Kevin Mohatt for The New York Times“We have a very finite amount of time,” said Dr. Anne Zink, the chief medical officer for Alaska. “In Alaska, kids go to the wind as soon as summer hits, so our opportunity to get them is now.”A number of places are revving up vaccination efforts in schools. In Colorado, Denver Health will expand clinics it operates in six public schools to middle school students. For the last few weeks, it has provided 150 to 400 vaccines every Saturday and Sunday, reaching not just high school juniors and seniors but sometimes their parents and older siblings, too.“It’s been really successful because we are doing it in their communities, where the kids are familiar,” said Dr. Sonja O’Leary, the medical director for Denver Health’s school-based health centers.Other states believe pediatricians’ and family doctors’ offices will be the best places to catch teenagers — and children as young as infants as companies plan eventually to seek authorization for the shots to be given to the youngest children. Until recently, few doctors had vaccines on hand for patients. But in recent weeks, the Centers for Disease Control and Prevention has made a major push to enroll pediatricians to give the shots.The thinking is that pediatricians are in the best position to field questions from parents and children. Not only are they experienced in giving routine childhood vaccinations, but they are also often a household’s most trusted source of health information.President Biden announced plans last week to ship doses of the Pfizer vaccine directly to pediatricians’ offices, and he said that about 20,000 pharmacy sites were also ready to administer the vaccine to younger adolescents.There are also practical issues. Staggering Covid shots around the routine vaccines required for school in September — which many children are behind on because of the pandemic — will be complicated. According to the C.D.C., no vaccines can be given two weeks before and after a Covid vaccine.Pediatricians are used to talking to nervous parents about vaccines, but they concede that the Covid shot poses unique persuasion challenges. To help these conversations, the American Academy of Pediatrics has posted answers to frequently asked questions and has been holding virtual training workshops.Pediatricians say they have been getting vaccine questions for months.From left, Garrett Bates, his sons Christopher Bates and Preston Janac; Precious Wright, his partner; and his daughter Tyshawnie Bates, of Hollywood, Fla.Octavio Jones for The New York TimesMany parents and teenagers have been stirred by false information coursing across the internet about the shots’ impact on fertility and menstrual cycles, said Dr. Hina Talib, an adolescent medicine specialist at Children’s Hospital at Montefiore Medical Center in the Bronx, who posts on Instagram as @teenhealthdoc.“With hormones floating around during puberty, parents ask if it’s dangerous for their child to be given a vaccine during that time,” Dr. Talib said. The questions reflect the parents’ thoughtfulness, she said, and need to be addressed respectfully.Dr. Talib, whose patients are often Black or Latino and recent immigrants, said that many hear vaccine resistance at home. “We have to validate parental anxiety and mistrust of medicine and be very open to listening to what their experiences have been,” she said.Garrett Bates and Precious Wright, who live in Hollywood, Fla., have tentatively decided to get themselves vaccinated, but they are holding off on their four children, ages 12 through 19, just now.It has been a tough year: Two of the children attended school in person, two were remote. Yet, even though vaccination offers the possibility that all their children will have a more engaged, carefree life, Ms. Wright wants to see how others their age fare first.“From what I know, you take the vaccine and some people feel sick and it lasts a couple of hours or a day,” she said. “My immune system is stronger than the kids’. I don’t know if they could shake off those effects as quickly as mine.”For some teenagers, anxious about bringing the virus home to vulnerable relatives, the vaccine represents liberation — from those worries as well as constraints on seeing friends.“The kids have ‘shot envy,’” Dr. Talib said.Dr. Nicole Baldwin, a pediatrician in Cincinnati whose health-related TikTok videos now feature one for the Pfizer vaccine, said she was surprised by how excited many of her teenaged patients were about the vaccine. “I’ll ask, ‘Have your friends gotten it?’ And they’re saying, ‘Yes!’”But she also has patients, including those with high-risk medical conditions that make them vulnerable to Covid, who are not getting it. “Their parents say no,” she said.When parent and child are at odds about the vaccine, the pediatrician has a tricky path to walk. And when divorced parents disagree over whether their child should get the vaccine, those discussions become even more difficult.Not all teenagers long for the vaccine. Many hate getting shots. Others say that because young people often get milder cases of Covid, why risk a new vaccine?Patsy Stinchfield, a nurse practitioner who oversees vaccination for Children’s Minnesota, has stark evidence that some cases in young people can be serious. Not only have more children with Covid been admitted to the hospital recently, but its intensive care unit also has Covid patients who are 13, 15, 16 and 17 years old.The F.D.A.’s new authorization means all those patients would be eligible for the shots, she noted. “If you can prevent your child ending up in the I.C.U. with a safe vaccine, why wouldn’t you ?” she said.Mr. Quesnel, the East Hartford, Conn., superintendent, said the most powerful message for reaching older adolescents would probably appeal just as much to younger ones. Rather than focusing on the fact that the shot will protect them, he said, they seize on the idea that it will keep them from having to quarantine if they are exposed.“They’re not so afraid of the health care dangers from Covid but the social losses that come along with it,” he said, adding that 60 percent of his district’s seniors, or about 300 students, got their first dose at a mass vaccination site run by Community Health Center on April 26. “Some of our greatest leverage right now is that social component — ‘You won’t be quarantined.’”Michael Jackson of North Port, Fla., can’t wait for his 14-year-old son, Devin, to get the vaccine. During the past year, he said, his son’s beloved Little League games went on hiatus and the family had to suspend their regular Sunday suppers with grandparents And Devin, an eighth grader, had to quarantine three times after being exposed to Covid.Other parents have challenged Mr. Jackson about his plans to get Devin vaccinated. “They say to me, ‘How can you put that in your body?’” he said, adding, “And meanwhile they’re eating a Big Mac and drinking a can of soda?”Michael Jackson, left, of North Port, Fla., is eager for his 14-year-old son, Devin, to get vaccinated.Octavio Jones for The New York TimesBefore any younger adolescents can receive the shots, the C.D.C.’s vaccine advisory committee will meet in the coming days to review the clinical trial data and make recommendations for the vaccine’s use in the 12-to-15 age group.Within months, eligibility for the vaccines is expected to expand to even younger children. Pfizer expects to seek emergency authorization in September to administer its vaccine to children between the ages of 2 and 11. Moderna’s clinical trial results for its vaccine in 12- to 17-year-olds are expected in the next few weeks, and those from a trial of its vaccine in children 6 months to 12 years old in the second half of this year.All 50 states require certain vaccines for children who attend school, but those mandates apply only to vaccines that have been fully approved by the F.D.A., a status the Covid shots have not yet achieved. And even when the F.D.A. approves the vaccines, any state-legislated mandates would most likely allow students to opt out for medical, religious and sometimes even philosophical reasons, as they do for other childhood shots.In Columbus, Dr. Roberts already has a good sense of the challenge ahead. Her department worked with the local children’s hospital to offer vaccinations to older teenagers at high schools over the last month, hoping to reach up to 6,000 of them.“We only got about 600,” she said, noting that parental fears about infertility were the most common reason for refusing the shots. Now she and her staff are considering offering incentives like free meals and grocery store gift cards to parents, and perhaps prizes for children as well.“We’re committed to getting this population vaccinated,” she said, “so we’re going to look at anything and everything.”
Read more →