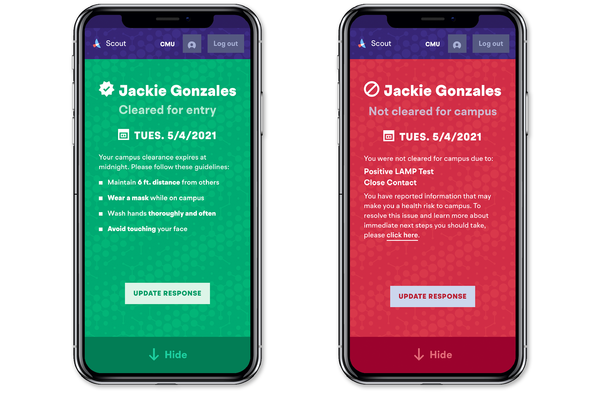
One weekend last August, Shynell Moore woke up with a headache and a sore throat. Ms. Moore, then just a few weeks into her junior year at Colorado Mesa University, pulled out her phone and fired up a symptom-tracking app called Scout.Within seconds of reporting her symptoms, the screen turned red: She might have Covid-19, the app said. She promptly got a call from a school administrator, and before the day was out, she had packed some clothes and her elephant ear fish, Dumbo, and moved into quarantine housing. Her Covid-19 test soon came back positive.Several days into her quarantine period, Ms. Moore took a whiff of Dumbo’s typically malodorous food. “I couldn’t smell it,” she said. “And then I drank some cough syrup, and I couldn’t taste it.” She opened Scout and clicked an option: “Lost taste or smell.”Students at Colorado Mesa University use the Scout app to report symptoms.Fathom/C.M.U.Each time she reported a symptom, the information was transmitted to Lookout, the university’s digital Covid-19 dashboard. Over the months that followed, Lookout evolved into a sophisticated system for tracking Covid-19 symptoms and cases across campus, recording students’ contacts, mapping case clusters, untangling chains of viral transmission and monitoring the spread of new variants.“Colorado Mesa has the most sophisticated system in the country to track outbreaks,” said Dr. Pardis Sabeti, a geneticist at the Broad Institute of M.I.T. and Harvard who has helped health officials around the world respond to Ebola, Lassa fever and other infectious diseases. “It’s definitely the kind of analytics that people talk about having but nobody actually has access to in this way.”Lookout is the product of a partnership between C.M.U. — a medium-sized school that sits in the high desert of Western Colorado and prides itself on serving disadvantaged students — and the Broad Institute, a cutting-edge genomic research center in Cambridge, Mass.Together, they have turned C.M.U.’s campus of 10,000-plus students into a real-world, real-time epidemiological laboratory, experimenting with creative approaches to pandemic management. Not everything has gone perfectly — college students will be college students, after all, and a university cannot be entirely cordoned off from the wider world. But the lessons they have learned and the tools they have developed could help institutions around the world better manage future outbreaks, Dr. Sabeti said: “We’re trying to build technologies that can be used globally. But a school is a great place to start.”Shynell “Nelly” Moore, a junior at Colorado Mesa University, contracted Covid-19 last fall and had to quarantine in the covid dorm. She brought her fish, Dumbo, with her.Eliza Earle for The New York TimesFacebook for outbreaksIn 2016 and 2017, mumps outbreaks blossomed across Massachusetts, hopping from one college campus to another. Dr. Sabeti worked closely with state epidemiologists, watching them map case clusters by hand and log data in increasingly unwieldy Excel spreadsheets. It was painstaking, time-consuming work, and the insights were “really hard-earned,” she said.In the years that followed, Dr. Sabeti and her postdoctoral fellow Andrés Colubri worked with a local firm, Fathom Information Design, to develop a symptom-tracking and contact-tracing app that could be used in future outbreaks. They imagined a scenario in which a college student could report a fever and then be informed that two students down the hall had recently developed the same symptom. “We called it the Facebook app for outbreaks,” Dr. Sabeti said.They were still developing the app, which became Scout, when Covid-19 hit. “Five-year plans turned into six-month plans,” Dr. Sabeti said. Fathom raced to finish the app, while Dr. Sabeti looked for a place to pilot it.Dr. Pardis Sabeti, a geneticist at the Broad Institute of M.I.T. and Harvard, has helped health officials around the world respond to Covid-19, Ebola, Lassa fever and other infectious diseases.Damon Winter/The New York TimesShe had begun advising colleges across the country on their coronavirus responses, but C.M.U., based in Grand Junction, Colo., immediately stood out to her. “We were looking for somebody who was scrappy, hungry, ready to go,” Dr. Sabeti said. “And we felt there was a need there.”Like many schools, C.M.U. had suddenly suspended its in-person classes in mid-March 2020. College students everywhere were facing the same educational disruption. But C.M.U. administrators worried that their students — two-thirds of whom were students of color, low-income or the first in their families to go to college — might be permanently derailed by a semester, or longer, spent entirely online.And so the administration made a decision: In the fall, it would bring students back to campus. All of them. “It became really obvious very quickly, this was a moral imperative,” said John Marshall, the school’s vice president. “We had to find a way to get back.” (Mr. Marshall, himself a C.M.U. alumnus, was recently named the university’s new president, starting on July 1.)Mr. Marshall and Amy Bronson, who directs C.M.U.’s physician assistant program, became co-chairs of the campus coronavirus response. When they first connected with Dr. Sabeti in the summer of 2020, they told her about C.M.U.’s can-do, community spirit and their determination not to make it a “less than” year for students. They also sent her a music video that students had made about returning to campus safely. John Marshall, vice-president of C.M.U., and Amy Bronson, director of the university’s physician assistant program.Eliza Earle for The New York TimesAs the teams began to talk, it soon became clear that their work together would go far beyond piloting an app. They strategized about testing, planned for worst-case scenarios and devised new learning experiences, including a for-credit seminar, “Leaning In: Leadership in the Time of a Pandemic.” (Dr. Sabeti and the governor of Colorado were both guest lecturers.)“C.M.U. had this really bold desire to be back and to revive in-person education,” said Kian Sani, special projects adviser to Dr. Sabeti. “So we really put our entire team and effort into supporting that mission.” The teams just clicked, he said. “It was basically like, ‘Let’s all hold hands’ — without actually all holding hands, because it’s a pandemic.”All in the ‘mavily’When students returned in August, Scout became their campus wellness passport. Every day, they used Scout to report whether they had any Covid-19 symptoms or had recently traveled outside the area. (They were also encouraged to log the names of any recent close contacts.) If they had no symptoms and no recent travel, the screen turned green. This green screen was their ticket to enter the classroom, the cafeteria and other campus buildings. It quickly became a new daily habit for students. “It’s an every day thing, for sure,” Ms. Moore said. “It’s engraved in the head: Got to do it every day.”The data was fed into Lookout, the dashboard that Fathom had developed to give administrators a holistic view of what was happening on campus: “Across this 10,000-student population, how are we actually doing day to day?” said Fathom’s founder, Ben Fry, who built Scout and Lookout with his colleague Olivia Glennon.C.M.U. uses a dashboard called Lookout to track Covid-19 symptoms and cases across campus. (All screenshots show simulated data and names.)Fathom/C.M.U.In addition to aggregating symptom data, Lookout also pulls in hourly results from the university’s coronavirus testing site. The university, which did not have the resources to test every student every week, had created a tiered testing strategy. Taking inspiration from the school mascot, the Maverick, C.M.U. asked students to sort themselves into family units, or “mavilies,” that encompassed their regular close contacts.The university randomly selected 250 students to take a coronavirus test every week. But students in certain high-risk mavilies — like members of sports teams, who often practiced, ate and lived together — were selected more frequently than those in lower-risk ones.When a student tested positive, administrators could use Lookout to see who was in their mavily and any other recent contacts they had reported in Scout. Lookout also displayed a list of every mavily with a recent positive test result, as well as any “high-spread” mavilies with multiple recent positives. (Mr. Marshall, Dr. Bronson and the university’s lead contact tracer were the only people with access to the full dashboard; all publicly reported information was aggregated, rather than tied to individual students, Dr. Bronson said.)Lookout can show Covid-19 tests results within a dorm, a sports team or a “mavily,” a group of close student contacts.Fathom/C.M.U.If it seemed like the virus was beginning to spread within a mavily, which happened on the football team in September, the university could take quick action. “That was something that was really successful for us: Being able to say, in real time, ‘OK, we’re going to shut down operations protocols for your team to meet, and instead, a percentage of you are all going to go test,’” Dr. Bronson said. “And we’re going to know pretty quickly whether or not that is moving through the mavily.”Wastewater warningsEngineering students collecting wastewater samples to test for coronavirus on campus. They meet three times a week to conduct the sampling rounds.Eliza Earle for The New York TimesLookout also displays a geographic heat map of cases, a dorm view with room-by-room maps of positive and negative test results, and data from a new wastewater surveillance system, which tracks the coronavirus levels in the sewage flowing from various dorms. (People with Covid-19 shed the virus in their stool.) “As Lookout came together, it took this really complicated web of data and helped us start to both visually see it and to start making sense of it,” Mr. Marshall said.The wastewater data has proved critical. In late September, for instance, the team noticed a sudden spike in the viral levels in wastewater from Grand Mesa, a suite-style residence hall. They responded by strategically testing a subset of residents, making sure to get at least one from each suite or mavily. They found two positives, traced their contacts and sent the infected students into quarantine.But when the next wastewater readings came in from Grand Mesa, the viral level was still high. More testing and tracing revealed that some students had not been entirely honest with the contact tracers about their social activities. The university ultimately identified four more cases in the dorm.Wastewater samples can help identify dorms that need additional Covid-19 testing.Fathom/C.M.U.“The kids were telling us one thing, but the data was telling us something different,” Mr. Marshall said. “If you just paid attention to the testing and the tracing, you would say, ‘Right, we fixed it.’ But the wastewater data was telling us, ‘Nope, you haven’t fixed it, you better go back in.’ And it allowed us to ultimately keep that confined.” (Despite some isolated incidents of dishonesty, most students cooperated with contact tracers, administrators said.)It was one of five times that the wastewater helped them discover multiple infected students in a particular dorm during the fall semester. “We feel pretty confident that we stopped five outbreaks,” said Kari Sholtes, an environmental engineer at C.M.U. who set up the wastewater system.C.M.U. is not the only school doing wastewater surveillance or targeted testing. But what sets C.M.U. apart is how effectively it has combined all the available tactics, said Eric Parrie, the chief executive of COVIDCheck Colorado, a social enterprise company that has helped schools and organizations across the state — including C.M.U., 14 other universities and 33 school districts — implement their testing and vaccination programs. “I think it’s best in class,” he said. “I think that’s true in Colorado, and I think it’s probably true, actually, if you look across the country.”Outbreak operationsThe wastewater sampling crew with its testing gear making its way to another sampling site.Eliza Earle for The New York TimesWhile administrators were scrambling to stop outbreaks, students in the leadership seminar were working to simulate one, partnering with a Broad Institute team on “Operation Outbreak.”The campuswide simulation deployed an educational smartphone app, which Dr. Sabeti and Dr. Colubri had developed several years prior. (Dr. Colubri now has his own lab at University of Massachusetts Medical School.) Over the Halloween weekend, hundreds of C.M.U. students went about their lives while letting the app, which could “transmit” a virtual virus to other nearby phones, run in the background. If students were in close proximity to another participating phone, they might become “infected.”The goal was to “empower the students to better understand how their actions are influencing their community and influencing their friend groups,” said Bryn Loftness, a C.M.U. computer science major who helped lead the project. “Maybe they’ll find out through this app that ‘Oh, I wasn’t social distancing as much as I thought I would, and I had this many close contacts. Maybe I can do better.’” (Ms. Loftness, who graduated from C.M.U. at the end of that semester, currently works as a research intern in Dr. Sabeti’s lab.)The data revealed that while many students were being careful, there was a subset with a lot of social contacts — maybe even enough of them to fuel a larger outbreak..css-1xzcza9{list-style-type:disc;padding-inline-start:1em;}.css-3btd0c{font-family:nyt-franklin,helvetica,arial,sans-serif;font-size:1rem;line-height:1.375rem;color:#333;margin-bottom:0.78125rem;}@media (min-width:740px){.css-3btd0c{font-size:1.0625rem;line-height:1.5rem;margin-bottom:0.9375rem;}}.css-3btd0c strong{font-weight:600;}.css-3btd0c em{font-style:italic;}.css-akgeos{margin-bottom:15px;font-family:nyt-franklin,helvetica,arial,sans-serif;font-size:0.75rem;line-height:1rem;color:#787878;}@media (min-width:740px){.css-akgeos{font-size:0.8125rem;line-height:1.125rem;}}.css-w739ur{margin:0 auto 5px;font-family:nyt-franklin,helvetica,arial,sans-serif;font-weight:700;font-size:1.125rem;line-height:1.3125rem;color:#121212;}#NYT_BELOW_MAIN_CONTENT_REGION .css-w739ur{font-family:nyt-cheltenham,georgia,’times new roman’,times,serif;font-weight:700;font-size:1.375rem;line-height:1.625rem;}@media (min-width:740px){#NYT_BELOW_MAIN_CONTENT_REGION .css-w739ur{font-size:1.6875rem;line-height:1.875rem;}}@media (min-width:740px){.css-w739ur{font-size:1.25rem;line-height:1.4375rem;}}.css-9s9ecg{margin-bottom:15px;}.css-1jiwgt1{display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-box-pack:justify;-webkit-justify-content:space-between;-ms-flex-pack:justify;justify-content:space-between;margin-bottom:1.25rem;}.css-8o2i8v{display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-flex-direction:column;-ms-flex-direction:column;flex-direction:column;-webkit-align-self:flex-end;-ms-flex-item-align:end;align-self:flex-end;}.css-8o2i8v p{margin-bottom:0;}.css-12vbvwq{background-color:white;border:1px solid #e2e2e2;width:calc(100% – 40px);max-width:600px;margin:1.5rem auto 1.9rem;padding:15px;box-sizing:border-box;}@media (min-width:740px){.css-12vbvwq{padding:20px;width:100%;}}.css-12vbvwq:focus{outline:1px solid #e2e2e2;}#NYT_BELOW_MAIN_CONTENT_REGION .css-12vbvwq{border:none;padding:10px 0 0;border-top:2px solid #121212;}.css-12vbvwq[data-truncated] .css-rdoyk0{-webkit-transform:rotate(0deg);-ms-transform:rotate(0deg);transform:rotate(0deg);}.css-12vbvwq[data-truncated] .css-eb027h{max-height:300px;overflow:hidden;-webkit-transition:none;transition:none;}.css-12vbvwq[data-truncated] .css-5gimkt:after{content:’See more’;}.css-12vbvwq[data-truncated] .css-6mllg9{opacity:1;}.css-1rh1sk1{margin:0 auto;overflow:hidden;}.css-1rh1sk1 strong{font-weight:700;}.css-1rh1sk1 em{font-style:italic;}.css-1rh1sk1 a{color:#326891;-webkit-text-decoration:underline;text-decoration:underline;text-underline-offset:1px;-webkit-text-decoration-thickness:1px;text-decoration-thickness:1px;-webkit-text-decoration-color:#ccd9e3;text-decoration-color:#ccd9e3;}.css-1rh1sk1 a:visited{color:#333;-webkit-text-decoration-color:#ccc;text-decoration-color:#ccc;}.css-1rh1sk1 a:hover{-webkit-text-decoration:none;text-decoration:none;}And then, just after the simulation ended, they had one.Over the course of October, the number of Covid-19 cases in the surrounding community, Mesa County, had climbed steadily. University officials watched with some trepidation; 90 percent of C.M.U. students had jobs, many in the service industry.Grace Tandus, left, and Madelyn Schmidt prepared for going out to collect samples.Eliza Earle for The New York TimesFor three weeks, it seemed like their pandemic measures might be enough to keep the virus off campus. But then, in early November, more cases began popping up at C.M.U. — in many different mavilies and dorms. Cases ticked up from 26, in the last week of October, to 124 the following week. The week after that, cases peaked at 290.The university tripled the size of its contact-tracing staff and quadrupled the number of tests it was administering. “We were, hour by hour, working through the contact tracing, working through the case management, watching wastewater,” Mr. Marshall said.As different mavilies became viral hot spots, administrators began implementing “Covid timeouts,” asking all members to follow a modified quarantine procedure until they found every affiliated case. They also urged students to be socially responsible, especially as they prepared to leave campus for Thanksgiving.To reduce student travel, C.M.U. had always planned to conduct virtual classes between Thanksgiving and winter break. Ultimately, it suspended in-person classes several days early to give students more time to get tested and isolate before returning home. “We did not send a bunch of people out of here, all positive, going to spread it to other places,” Dr. Bronson said.And when students left campus, C.M.U. opened its testing site to members of the broader community, who sometimes faced long waits at the county’s single drive-through testing site. “They helped ease that pressure,” said Jeff Kuhr, the executive director of Mesa County’s public health department. Over the next two months, C.M.U.’s testing site administered more than 18,000 tests to local residents. The autumn surge was “overwhelming,” Dr. Kuhr said. “But it was great to have C.M.U. by our side.”Life goes onLucas Torres, a biology major graduating on Saturday, had initially been nervous about returning to C.M.U. during a pandemic. But returning turned out to be a bright spot.Eliza Earle for The New York TimesThe November outbreak had illustrated how intertwined the university was with the wider community. So when students returned to campus in January, C.M.U. expanded mavilies, contact tracing and targeted testing efforts to include students’ off-campus contacts.The campus testing site remained open to all county residents. This “altruistic” testing strategy has become a cornerstone of the university’s response, and Dr. Sabeti’s team recently created a model demonstrating that this approach can help institutions keep their own members safe.The Broad Institute scientists have also begun sequencing Covid-19 tests and wastewater samples from C.M.U., identifying a new variant that spread rapidly across campus. Their collaborators are currently studying it to determine whether it might be more dangerous.The sequencing data — which is now, of course, in Lookout — has also allowed the teams to map hidden chains of transmission, identifying linked cases and providing hints about exactly when and where the virus is spreading.The Lookout dashboard can show sequencing data for confirmed cases.Fathom/C.M.U.So far, Mr. Marshall said, they have not identified a single case of coronavirus transmission that happened in the classroom, where students wore masks and remained socially distanced — and had to show a green screen for admission. Instead, most students seemed to contract the virus at small social gatherings or, to a lesser extent, in the workplace.The detailed, high-resolution data from C.M.U. will “help us better understand viral spread in congregate settings and how we can help mitigate it in the future,” said Dr. Sabeti, who plans to publish a “deep study” of the transmission dynamics at C.M.U.Aiming to gain the same sorts of insights, the Colorado Department of Public Health and Environment, is finalizing a deal to send samples from a few dozen state-run testing sites to the Broad Institute for sequencing, said Dr. Emily Travanty, the department’s lab director.Over the longer term, Dr. Sabeti and her colleagues hope to build versions of Scout and Lookout that can be used by schools, companies, local governments and other organizations around the world to respond to outbreaks of infectious disease.C.M.U. is also looking ahead, brainstorming about how they could adapt Scout for the fall, when many students will be vaccinated, and whether they can use their new tools to slow the spread of other infectious diseases, like flu. “We were on a call with Fathom a few days ago dreaming about what the long game looks like,” Dr. Bronson said.With graduation set for this weekend, Mr. Marshall, C.M.U.’s soon-to-be president, is pleased with how the past year has gone. “I view it as a success and not a small one,” he said. “I think we will look back on this year as being one of those defining moments for our university.” Yes, they had Covid-19 cases, he said, but they also had 881 freshmen who were the first in their families to go to college — who were able to actually go to college.“It was never about how do you stop a virus?” Mr. Marshall said. Instead, he said, the challenge was: “How do you manage life while dealing with a pandemic? And in that regard, I would say we’ve done as strong of a job as anybody.”Lucas Torres, a biology major graduating on Saturday, had initially been nervous about returning to C.M.U. during a deadly pandemic. And it had turned out to be an enormously difficult year for him: During winter break, he and several of his family members all got Covid-19. His mother developed pneumonia and his grandmother died from the disease.School had turned out to be a bright spot. Mr. Torres was “inspired” by C.M.U.’s response, he said: “It allowed for students to have a purpose. There was a responsibility, shared responsibility coming back to campus.”Shortly after recovering from Covid-19, he proposed to his girlfriend. (She said yes.) He is about to take his E.M.T. certification exam and hopes to go to medical school.“I was able to make the most of my time at C.M.U., and I’m glad that they allowed for that,” Mr. Torres said. “Even if it wasn’t the same as it would be if not for Covid, it was better than sitting at home in front of a screen.”
Read more →