Any high school reunion is a sharp reminder that some people age more gracefully than others. Some enter their older years still physically spry and mentally sharp. Others start feeling frail or forgetful much earlier in life than expected.
“The way we age as we get older is quite distinct from how many times we’ve traveled around the sun,” said Ahmad Hariri, professor of psychology and neuroscience at Duke University.
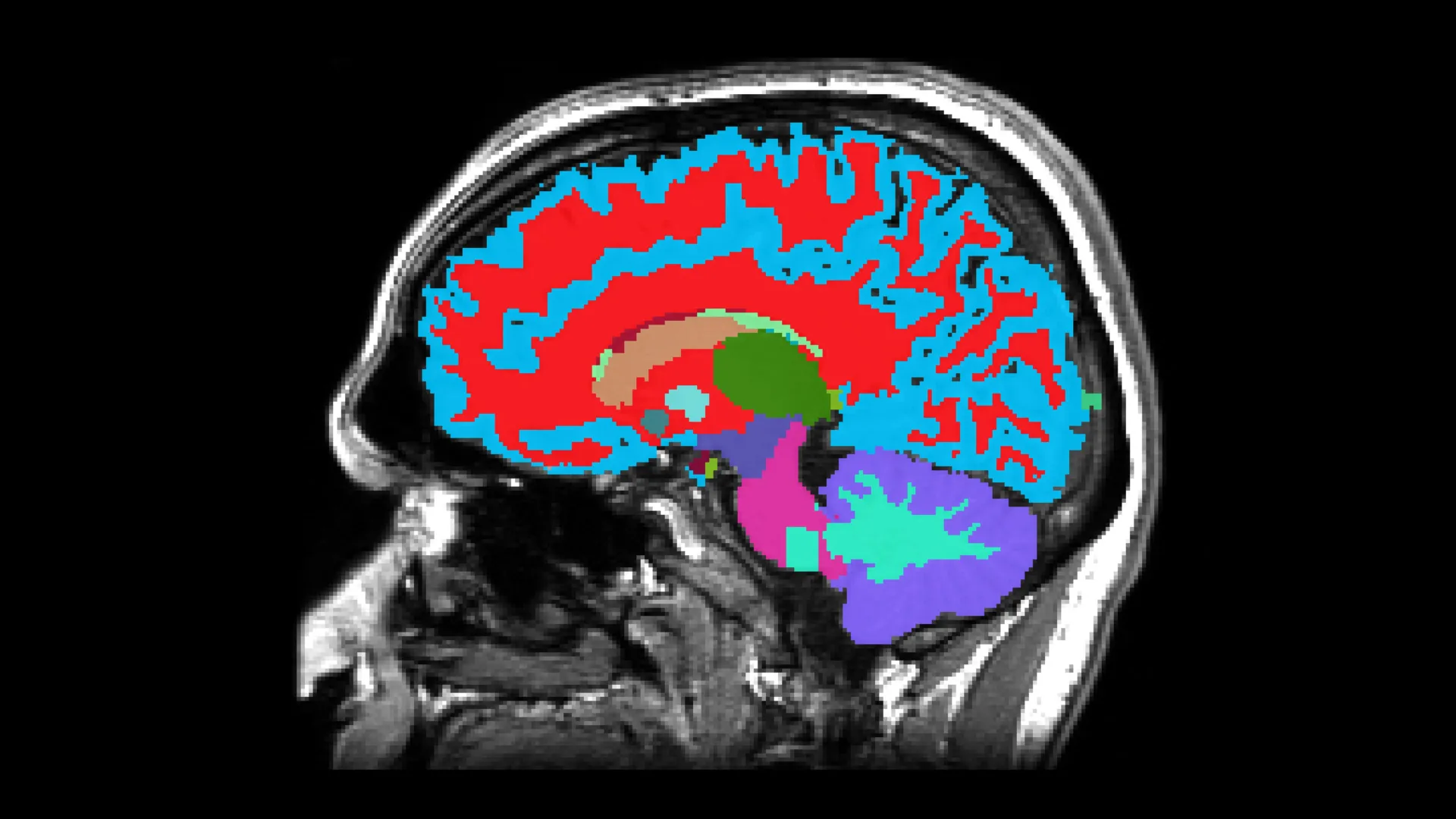
Now, scientists at Duke, Harvard and the University of Otago in New Zealand have developed a freely available tool that can tell how fast someone is aging, and while they’re still reasonably healthy — by looking at a snapshot of their brain.
From a single MRI brain scan, the tool can estimate your risk in midlife for chronic diseases that typically emerge decades later. That information could help motivate lifestyle and dietary changes that improve health.
In older people, the tool can predict whether someone will develop dementia or other age-related diseases years before symptoms appear, when they might have a better shot at slowing the course of disease.
“What’s really cool about this is that we’ve captured how fast people are aging using data collected in midlife,” Hariri said. “And it’s helping us predict diagnosis of dementia among people who are much older.”
The results were published July 1 in the journal Nature Aging.
Finding ways to slow age-related decline is key to helping people live healthier, longer lives. But first “we need to figure out how we can monitor aging in an accurate way,” Hariri said.
Several algorithms have been developed to measure how well a person is aging. But most of these “aging clocks” rely on data collected from people of different ages at a single point in time, rather than following the same individuals as they grow older, Hariri said.
“Things that look like faster aging may simply be because of differences in exposure” to things such as leaded gasoline or cigarette smoke that are specific to their generation, Hariri said.
The challenge, he added, is to come up with a measure of how fast the process is unfolding that isn’t confounded by environmental or historical factors unrelated to aging.
To do that, the researchers drew on data gathered from some 1,037 people who have been studied since birth as part of the Dunedin Study, named after the New Zealand city where they were born between 1972 and 1973.
Every few years, Dunedin Study researchers looked for changes in the participants’ blood pressure, body mass index, glucose and cholesterol levels, lung and kidney function and other measures — even gum recession and tooth decay.
They used the overall pattern of change across these health markers over nearly 20 years to generate a score for how fast each person was aging.
The new tool, named DunedinPACNI, was trained to estimate this rate of aging score using only information from a single brain MRI scan that was collected from 860 Dunedin Study participants when they were 45 years old.
Next the researchers used it to analyze brain scans in other datasets from people in the U.K., the U.S., Canada and Latin America.
Faster aging and higher dementia risk
Across data sets, they found that people who were aging faster by this measure performed worse on cognitive tests and showed faster shrinkage in the hippocampus, a brain region crucial for memory.
More soberingly, they were also more likely to experience cognitive decline in later years.
In one analysis, the researchers examined brain scans from 624 individuals ranging in age from 52 to 89 from a North American study of risk for Alzheimer’s disease.
Those who the tool deemed to be aging the fastest when they joined the study were 60% more likely to develop dementia in the years that followed. They also started to have memory and thinking problems sooner than those who were aging slower.
When the team first saw the results, “our jaws just dropped to the floor,” Hariri said.
Links between body and brain
The researchers also found that people whose DunedinPACNI scores indicated they were aging faster were more likely to suffer declining health overall, not just in their brain function.
People with faster aging scores were more frail and more likely to experience age-related health problems such as heart attacks, lung disease or strokes.
The fastest agers were 18% more likely to be diagnosed with a chronic disease within the next several years compared with people with average aging rates.
Even more alarming, they were also 40% more likely to die within that timeframe than those who were aging more slowly, the researchers found.
“The link between aging of the brain and body are pretty compelling,” Hariri said.
The correlations between aging speed and dementia were just as strong in other demographic and socioeconomic groups than the ones the model was trained on, including a sample of people from Latin America, as well as United Kingdom participants who were low-income or non-White.
“It seems to be capturing something that is reflected in all brains,” Hariri said.
The work is important because people worldwide are living longer. In the coming decades, the number of people over age 65 is expected to double, reaching nearly one fourth of the world’s population by 2050.
“But because we live longer lives, more people are unfortunately going to experience chronic age-related diseases, including dementia,” Hariri said.
Dementia’s economic burden is already huge. Research suggests that the global cost of Alzheimer’s care, for example, will grow from $1.33 trillion in 2020 to $9.12 trillion in 2050 — comparable or greater than the costs of diseases like lung disease or diabetes that affect more people.
Effective treatments for Alzheimer’s have proven elusive. Most approved drugs can help manage symptoms but fail to stop or reverse the disease.
One possible explanation for why drugs haven’t worked so far is they were started too late, when the Alzheimer’s proteins that build up in and around nerve cells have already done too much damage.
“Drugs can’t resurrect a dying brain,” Hariri said.
But in the future, the new tool could make it possible to identify people who may be on the way to Alzheimer’s sooner, and evaluate interventions to stop it — before brain damage becomes extensive, and without waiting decades for follow-up.
In addition to predicting our risk of dementia over time, the new clock will also help scientists better understand why people with certain risk factors, such as poor sleep or mental health conditions, age differently, said first author Ethan Whitman, who is working toward a Ph.D. in clinical psychology with Hariri and study co-authors Terrie Moffitt and Avshalom Caspi, also professors of psychology and neuroscience at Duke.
More research is needed to advance DunedinPACNI from a research tool to something that has practical applications in healthcare, Whitman added.
But in the meantime, the team hopes the tool will help researchers with access to brain MRI data measure aging rates in ways that aging clocks based on other biomarkers, such as blood tests, can’t.
“We really think of it as hopefully being a key new tool in forecasting and predicting risk for diseases, especially Alzheimer’s and related dementias, and also perhaps gaining a better foothold on progression of disease,” Hariri said.
The authors have filed a patent application for the work. This research was supported by the U.S. National Institute on Aging (R01AG049789, R01AG032282, R01AG073207), the UK Medical Research Council (MR/X021149/1), and the New Zealand Health Research Council (Program Grant 16-604).
Read more →