‘As a GP I felt I had to work during my cancer scare’
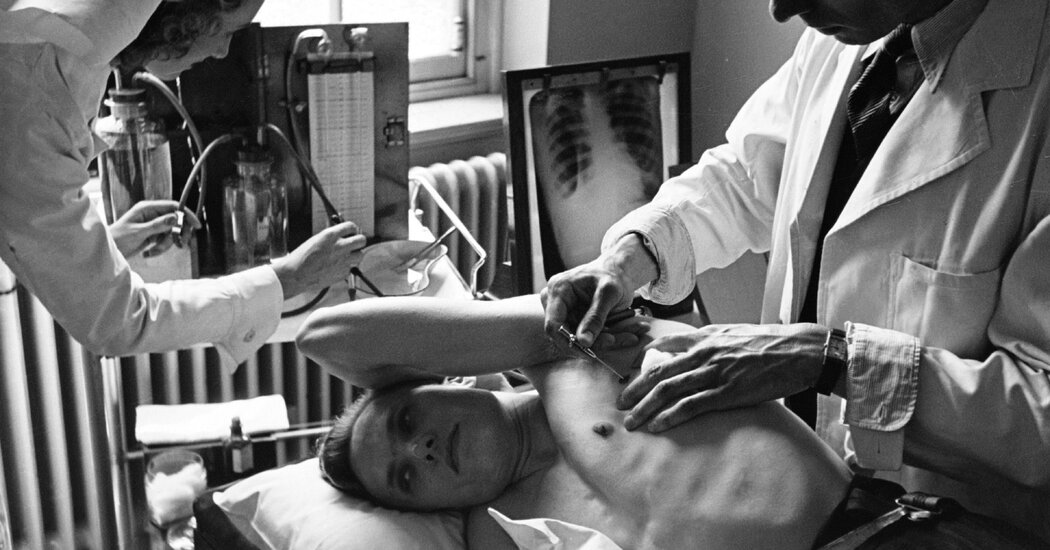
4 hours agoShareSaveTerel EdmundsBBC NewsShareSaveBBCA GP has said she kept on working through a cancer scare because otherwise her patients would not have been seen due to staffing issues made worse by funding.Dr Emily Jones is not alone feeling under pressure, as a colleague at their south Wales surgery worries she will make a mistake because she is seeing more patients than the recommended daily safe limit due to financial pressures.Some doctors claim these issues are made worse by an “outdated” health funding model which does not take into account how sick or poor a surgery’s catchment is.The Welsh government said parts of GP contracts, including funding formulas, would be considered as part of annual contract negotiations.The UK government has said it is reviewing the formula while the Welsh Parliament is looking at it as part of its inquiry into the future of GPs.”It puts the pressure on that I shouldn’t be getting sick,” Dr Jones said.The 37-year-old had nipped away from her practice to get an issue checked out and her doctor found a potentially cancerous lump in her abdomen.”My GP said that I should be going straight to the hospital,” she recalled.”But I couldn’t because I was the only doctor here, I couldn’t shut the surgery.”It was very stressful that afternoon trying to just keep going. I was in pain but there wasn’t really any other option.”Dr Jones said there was not enough staff to cover her that day because of a funding formula for GP surgeries in Wales and England that some say is no longer fit for purpose.When more doctors were in the following day, Dr Jones was able to attend the hospital appointment where the lump was found not to be cancerous.She said she has also felt awful taking time off to attend emergency hospital appointments and to have major operations because it put a strain on her surgery in Cardiff.”I hear quite a lot you don’t think about doctors getting sick, but I try to remind my patients that we’re all human,” added Dr Jones, a GP for eight years.Dr Rebecca TownerWhitchurch Road Surgery in the Heath area of the city currently has about 80 appointments a day for the approximate 8,000 patients on their list and has an estimated four-week wait for routine appointments. The surgery has said some staff are doing overtime every day to see as many patients as quickly as possible.”You have patient after patient coming in and the first five minutes is spent apologising for the fact they can’t get an appointment,” said Dr Rebecca Towner.The 44-year-old has said she could see 30 patients in a morning, which is beyond the safe daily limit of 25 suggested by the British Medical Association (BMA). The BMA said some GPs were seeing as many as 40 patients in a day due to an increased workload as some surgeries claim they cannot afford more doctors. “Every single day you worry you’re going to make a mistake,” added Dr Towner.”There’s more risk with seeing patient after patient and less time to think. We’re firefighting and it’s exhausting.”She has admitted the situation can be “demoralising” and doctors she knows have considered quitting multiple times. “I can’t imagine doing anything else other than being a GP, but it’s hard to see how we can carry on as it is at the moment,” added Dr Towner.Bosses at Whitchurch Road Surgery have put a cap on extra work “when possible” and claim a lack of funding because of the way the NHS pays GP surgeries means they have been unable to pay the same wages as other practices.They say that means they are unable to hire new staff which has added to their workload and subsequently increased appointment wait time for patients.The surgery’s own practice manager said he continued to work during his treatment for stage three oesophageal cancer in an attempt to lessen the impact on patients.”I think things will get worse before they get better,” said Gareth Lucocq, 47.”We have lots of doctors qualifying in autumn and unfortunately there are no jobs for them because practices can’t afford their wages.”GPs in Wales and England are mainly paid using a formula introduced in 2004, based on factors like how old and ill their patients are likely to be. Campaigners have said the data the Carr-Hill Formula uses is more than 25 years old and GP practices in towns and cities tend to lose out.Doctors complain the formula is not based on current data so when the NHS allocates cash, it does not take into account whether the GP surgery serves a particularly sick or deprived population.BBC Wales research shows that if Whitchurch Road Surgery was paid per patient, rather than using the Carr-Hill formula, it would receive an extra quarter of a million pounds a year.Based on this measurement, the biggest shortfall faced by any GP surgery in Wales would be just under £445,000.”There is systematically worse access to general practice in poorer parts of the country,” said Dr Becks Fisher of the Nuffield Trust, who did a study on the GP funding formula in England.”People who live in poorer parts of the country consistently have lower satisfaction with GP services and report more difficulty in accessing them.”GP practices in the Cardiff and Vale health board are the worst affected by the formula in Wales and almost half of Welsh surgeries claim they are allocated less cash than they say they need.”If you’re hundreds of thousands of pounds worse off, it doesn’t matter how hard you work,” said Dr Matthew Jones, who works at another surgery in Heath.”The formula just doesn’t work. It doesn’t accurately represent what your GP workload is and the figures and data they’re using are from 1998 to 2001.”The General Practitioners Committee, the body that represents UK GPs, believes there is a need to review the formula in Wales.”General practice is facing a crisis in Wales,” said Dr Gareth Oelmann, the BMA’s Welsh committee chair.The Royal College of General Practitioners has welcomed the “long overdue” UK government review into how funds are dished out to GP surgeries.”A patient’s postcode and where they live should not determine the level of NHS care they receive,” it said in a statement.”It can’t be right that people in deprived communities – who often have more complex health needs and would likely benefit from health interventions most – are less likely to receive it, because their GPs’ time is spread even more thinly.”In Wales, the Senedd’s Health and Social Care Committee is holding an inquiry into the future of GPs including its funding model and current financial pressures.”Various elements of the GP contract, including funding formulas, will be considered as part of annual contract negotiations between Welsh government, NHS Wales and the General Practitioner’s Committee,” the Welsh government said in a statement.
Read more →