This new drug candidate might finally outsmart tuberculosis
Scientists have created a promising new compound that could mark a major step forward in the global effort to control tuberculosis, the world’s deadliest infectious disease.
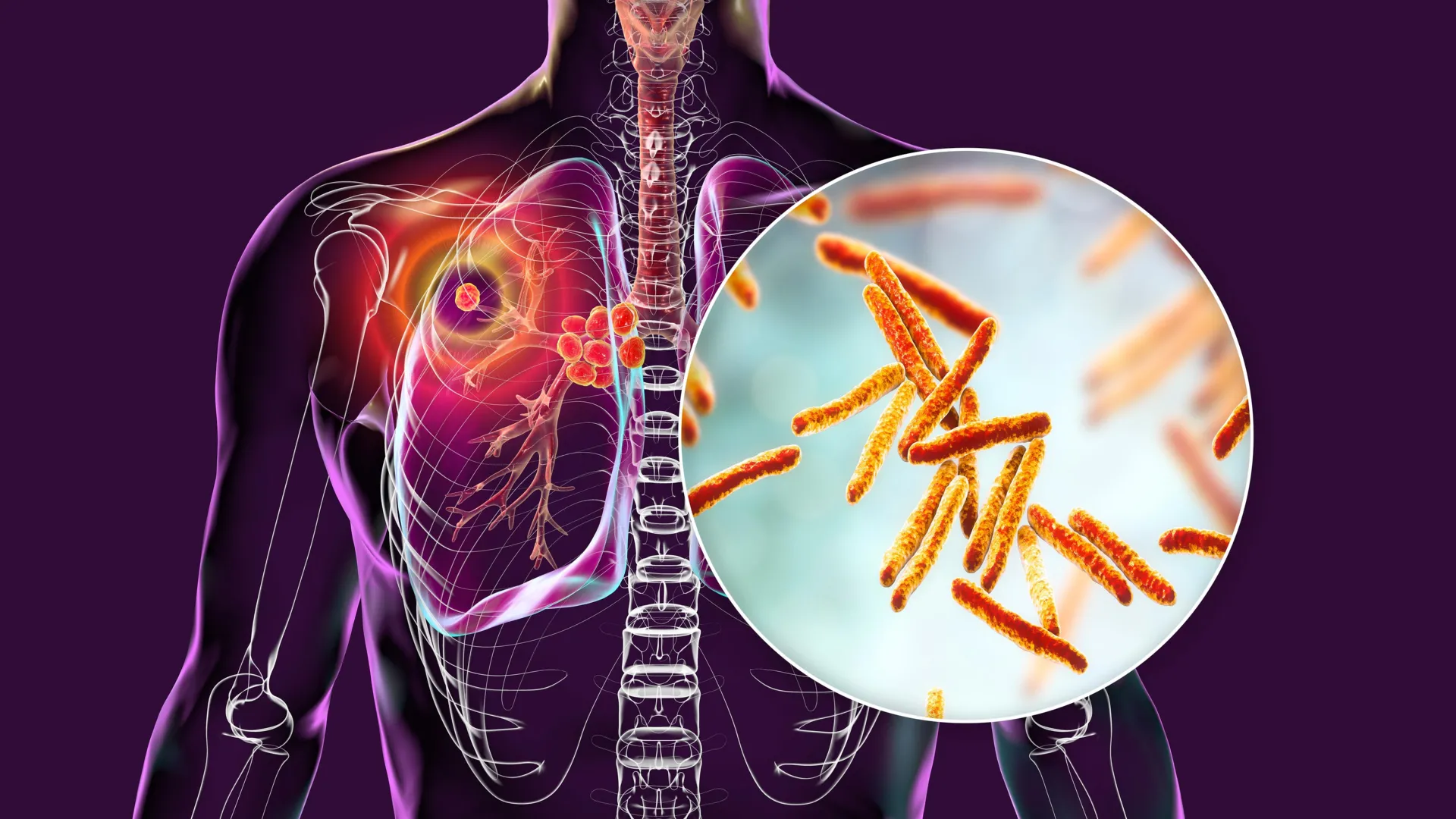
A new study in Nature highlights the potential of this compound, called CMX410, which targets a key enzyme in Mycobacterium tuberculosis, the bacterium that causes tuberculosis. The compound has shown success even against drug-resistant strains, a growing global problem that makes treatment more difficult and less effective.
The research was led by James Sacchettini, Ph.D., the Rodger J. Wolfe-Welch Foundation Chair in Science and professor at Texas A&M University, along with Case McNamara, Ph.D., senior director of infectious disease at the Calibr-Skaggs Institute for Innovative Medicines, a division of Scripps Research that develops next-generation therapies.
This discovery emerged from collaborations within the TB Drug Accelerator program, a Gates Foundation-funded initiative that brings together researchers to advance the most promising tuberculosis treatments.
“A lot of people think of tuberculosis as a disease of the past,” Sacchettini said. “But in reality, it remains a major public health issue requiring significant attention, collaboration and innovation to overcome.”
A new approach to an old enemy
The newly identified compound from AgriLife Research and Calibr-Skaggs works by shutting down a vital enzyme, polyketide synthase 13 (Pks13), which the bacterium needs to build its protective cell wall. Without this structure, M. tuberculosis cannot survive or infect the body.
Scientists have long known that Pks13 is an important target for TB drugs, but developing a safe and effective inhibitor has proven difficult. CMX410 succeeds where earlier attempts fell short. Its design makes it extremely specific to its target, resulting in fewer unwanted effects. The compound forms an irreversible bond with a critical site on Pks13, which prevents resistance from developing and keeps the drug focused on its intended target.
To achieve this, researchers used a technique known as click chemistry — a method that links molecules together like puzzle pieces. The approach was pioneered by co-author Barry Sharpless, Ph.D., W.M. Keck Professor of Chemistry at Scripps Research and a two-time Nobel Laureate. His work has opened the door to vast libraries of chemical compounds that can be rapidly tested and refined.
“This technique represents a new tool for drug design,” said McNamara. “We expect to see its uses expand in the coming years to help address public health concerns with a critical need, including tuberculosis.”
Promising early results
The team began by screening a collection of compounds from the Sharpless lab to find those capable of slowing M. tuberculosis growth. After months of optimization, led by co-first authors Baiyuan Yang, Ph.D., and Paridhi Sukheja, Ph.D., CMX410 emerged as the most effective and balanced candidate.
Yang’s team tested more than 300 variations to fine-tune the compound’s power, safety, and selectivity. The final version was tested against 66 different TB strains, including multidrug-resistant samples taken from patients, and proved effective in nearly all cases.
“Identifying this novel target was an exciting moment,” said Sukheja, who led many early studies showing CMX410 could target a previously unexplored gene. “It opened up a completely new path forward, especially against strains that have learned to evade existing treatments.”
The researchers also found that CMX410 can be used safely alongside existing TB drugs, a crucial advantage since treatment typically involves multiple medications taken for several months. In animal testing, no negative side effects were observed even at the highest doses. Because of its precision, the compound is unlikely to disturb healthy bacteria or cause gut imbalance — an issue often linked to traditional antibiotics.
Moving closer to better therapies
The addition of a specialized chemical group that allows CMX410 to permanently attach to its target makes it one of the most selective compounds of its kind. Although more studies are needed before it can be tested in humans, early findings suggest strong potential for future TB treatment.
“These early results are very encouraging,” said Inna Krieger, Ph.D., senior research scientist in Sacchettini’s lab and co-first author of the paper. “Cell wall-targeting antibiotics have long been a cornerstone of tuberculosis treatment. However, after decades of widespread use, their effectiveness is waning due to the rise of drug-resistant strains.
“We are working to discover new drugs that disrupt essential biological processes and identify optimal combinations with existing drugs to enable shorter, safer and more effective treatment regimens. Through these efforts, we hope to help move the world closer to a future free from tuberculosis.”