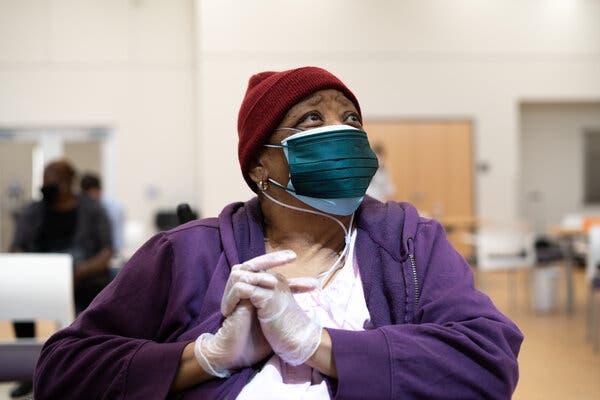
Some Elderly African Americans Are Hesitant About the Covid Vaccine
#masthead-section-label, #masthead-bar-one { display: none }The Coronavirus OutbreakliveLatest UpdatesMaps and CasesRisk Near YouVaccine RolloutNew Variants TrackerAdvertisementContinue reading the main storySupported byContinue reading the main story‘At Your Age, It’s the Vaccine or the Grave’A nurse in Baton Rouge has been on a crusade to overcome resistance among older African-Americans unwilling to take the coronavirus vaccine.Flossie West, 73, at the East Baton Rouge Council on Aging after receiving a shot of the coronavirus vaccine. “I’m just not interested because everyone tells me the virus is a hoax,” she had said earlier.Credit…Abdul Aziz for The New York TimesMarch 6, 2021, 1:52 p.m. ETBATON ROUGE, La — Flossie West was not at all interested in taking the coronavirus vaccine.Carla Brown, the nurse overseeing her care, was determined to change her mind.Ms. West, 73, has ovarian cancer, congestive heart failure and breathing difficulties — conditions that place her at grave risk should she contract the virus. As it is, Covid-19 has killed far too many of her neighbors in Mid-City, a low-rise, predominantly Black community that sprawls to the east of the Louisiana state capital.But Ms. West’s skepticism about the new vaccines overshadowed her fears of Covid-19. “I’m just not interested because everyone tells me the virus is a hoax,” Ms. West said. “And besides, that shot is going to make me more sick than I already am.”On Thursday morning, Ms. Brown, 62, breezed into Ms. West’s apartment and delivered a stern lecture: The virus is real, the vaccines are harmless and Ms. West should get out of bed, grab her oxygen tank and get into her car.“I’ll be darned if I’m going to let this coronavirus take you,” she said.In recent weeks, Ms. Brown has been frenetically working to persuade her patients to get inoculated, and her one-woman campaign provides a glimpse into the obstacles that have contributed to the troublingly low rates of vaccination in the Black community.Even as vaccine supplies become more plentiful, African-Americans are being inoculated at half the rate of whites, according to an analysis by The New York Times. The disparities are especially alarming given the disproportionate impact of the pandemic on communities of color, who have been dying at twice the rate of whites.Success! Flossie West received her first dose of the Moderna vaccine.Credit…Abdul Aziz for The New York TimesMs. Brown’s mission is fueled by personal loss. “My husband survived being shot in the head, and cancer twice, only to die from Covid-19,” she said. Credit…Abdul Aziz for The New York TimesThe racial gap in vaccination rates is no less stark in Louisiana, where African-Americans make up 32 percent of the population but just 23 percent of those who have been vaccinated.Part of the problem is access. In Baton Rouge, the majority of mass vaccination sites are in white areas of the city, creating logistical challenges for older and poorer residents in Black neighborhoods like Mid-City who often lack access to transportation. Older residents have also been thwarted by online appointment systems that can be daunting for those without computers, smartphones or speedy internet connections.But much of the racial disparity in vaccination rates, experts say, can be tied to a longstanding mistrust of medical institutions among African-Americans. Many Baton Rouge residents can readily cite the history of abuse: starting with the eugenics campaigns that forcibly sterilized Black women for nearly half of the 20th century, and the notorious government-run Tuskegee experiments in Alabama that withheld penicillin from hundreds of Black men with syphilis, some of whom later died of the disease.“The distrust among Black Americans comes from a real place and to pretend it doesn’t exist or to question whether it’s rational is a recipe for failure,” said Thomas A. LaVeist, an expert on health equity and dean of the School of Public Health and Tropical Medicine at Tulane University. Dr. LaVeist has been advising Louisiana officials on ways to increase vaccination rates.Seniors arrived at the East Baton Rouge Council on Aging to receive the vaccine.Credit…Abdul Aziz for The New York TimesRobbie Christian, a pharmacist, prepared to administer a dose of the Moderna vaccine at the Council on Aging. Credit…Abdul Aziz for The New York TimesMs. Brown, 62, the hospice nurse, has a good idea about how to change the minds of vaccine skeptics: encouraging one-on-one conversations with respected figures in the Black community who can address the misgivings and provide reliable information while acknowledging what she describes as the scars of inherited trauma. “If you look back at our history, we have been lied to and there has been a lot racial pain so it’s all about building trust,” she said.The Coronavirus Outbreak
Read more →