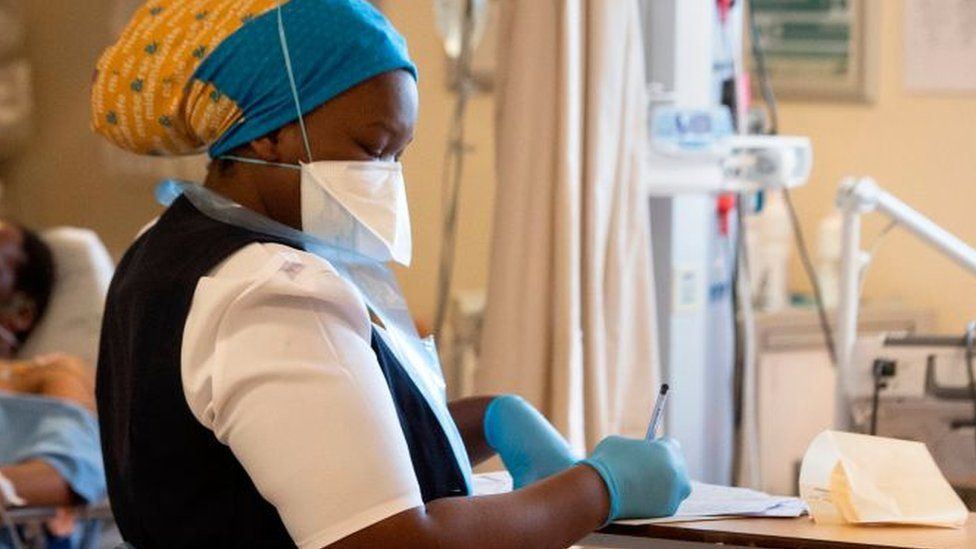
This phase of the pandemic, when adults can be vaccinated but young children cannot, is confusing for many families.Children playing at the U.S. National Arboretum in Washington last month. Public health experts say being outdoors is a safer way for children to socialize. Amr Alfiky/The New York TimesAs vaccinated Americans return to many parts of their prepandemic lives this summer, one group will be left out: children under 12, who cannot yet be vaccinated. So what should families with young children do when everyone else starts socializing again?We asked experts as part of an informal New York Times survey. The group of 828 who responded included epidemiologists, who study public health, and pediatric infectious disease physicians, who research and treat children sick with diseases like Covid-19.They noted that this phase was temporary. Pfizer has said vaccines for children ages 2 and up could come as soon as September. Of the survey respondents with young children, 92 percent said they would vaccinate their own children as soon as a shot was approved. (Only five said no; some were undecided.) In the meantime, families with young children may need to retain more precautions, like masking and distancing, than their childless friends do. But they said some minimally risky activities could help counteract the mental health effects of pandemic living.“Kids need to be able to be kids,” said Mac McCullough, an associate professor at Arizona State. “Outdoor activity isn’t perfectly safe, but its benefits are likely to outweigh its risks across an entire population.”We asked the experts about a few situations that families could encounter, and how they suggested parents and unvaccinated children should behave. There was no consensus, but they mostly advised weighing the relatively small health risks against the benefits of widening children’s worlds. As always, epidemiologists — who tend to be a very cautious group — emphasized that it would depend on the exact circumstances, and on local case rates.“I think a lot of families are frustrated and feel left out and anxious as to how to navigate life now,” said Dr. Sahera Dirajlal-Fargo, an infectious disease pediatrician at Case Western Reserve University. “Children have asked me, ‘Everyone else gets to move on, what about us?’ I am focusing on what we know families can do safely, and we know so much more than we did last year.”Here’s what they said.Indoor and crowded outdoor public placesNew guidance from the Centers for Disease Control and Prevention says that vaccinated people can go almost everywhere without a mask. But what should families with unvaccinated children do, since it’s impossible to know whether maskless people in public places are vaccinated? A slight majority said that despite that uncertainty, children could still go inside public places or be in outdoor crowds, as long as they wore masks. “As a mom, I’m not going to bring my children into such places if I can avoid it. But over all, I think the risk is very low, particularly if children wear masks.”Kelly Hirko, assistant professor, Michigan State University“Our children look to us — anywhere I would want them to mask, I’ll be masking as well, to set the example.”Corinne McDaniels-Davidson, director, San Diego State University Institute for Public Health“Huge problem here. The onus is now on children (and parents) to deal with and overcome problems generated from adults who refuse to get vaccinated (and likely won’t wear masks anymore).”Alan Kinlaw, assistant professor, University of North Carolina at Chapel HillIndoor social gatherings with other unvaccinated childrenVaccinated people can socialize indoors with one other household of unvaccinated people, the C.D.C. says. But what about two families getting together, when the adults are vaccinated but the children are not? The plurality of experts said two families with unvaccinated children could gather indoors, but should limit the number of families they see this way, like in a pod.“We will try to stay outdoors where possible, but will allow kids to be indoors without masks with a few select families.”Emily Henkle, research assistant professor of epidemiology, Oregon Health and Science University-Portland State University“With my unvaccinated children, we will not be socializing maskless indoors with other families with kids. My kids go to school and day care, and I am not willing to risk introducing Covid in those settings due to our family’s socialization activities.”Stina Mair, associate professor of behavioral and community health sciences, University of Pittsburgh“C.D.C. research has shown that schools have not been major sources of community transmission, but extracurricular activities are a different story. Unmasked activities among children should be limited to outdoor settings. When indoors, children should be masked.”Zack Hicks, epidemiology surveillance coordinator, Nebraska Department of Health and Human Services, 2019-20“This will not be easy to decide. For me, it will depend on the number of Covid-19 cases in my community and the latest data on the severity of the variants among children.”Laura Anderson, associate professor of health research, McMaster UniversityOutdoor activities where masks aren’t an optionUnvaccinated children are encouraged to continue wearing masks around other people, but there are some activities when that’s not possible. If they’re outdoors, and at low risk, it’s probably fine, eight in 10 said.“I think we need to make some sacrifices to have a more normal summer for our children. If we are outside, I think children will be able to eat and swim. When not doing those things directly, they should wear a mask.”Megan Benka-Coker, assistant professor of health sciences, Gettysburg College“I would not let my kids be in crowds of strangers who were not wearing masks, like in a crowded pool. I would ask them to wear a mask with other unvaccinated people, or keep distance when eating.”Ryan Carnahan, professor of epidemiology, University of IowaIndoor activities where masks aren’t an optionBut when it comes to indoor activities where masks cannot be worn at all times, children probably can’t safely do them this summer, three-quarters of the experts said.“There is a higher risk of acquiring the infection indoors. Also, as more variants emerge, some of them may be more serious for the children.”Asad Ansari, physician, Beacon Children’s Hospital“I fear these activities are what will drive the pandemic once adults are vaccinated.”Christopher J. Lehmann, physician and fellow for adult and pediatric infectious diseases, University of Chicago“Camps were able to safely open last summer with strict quarantine and testing protocols. I would encourage families to identify safe opportunities to get kids involved in these kinds of experiences. Eating inside a restaurant doesn’t seem like a necessary activity for children this summer.”Rosa Ergas, syndromic surveillance coordinator, Massachusetts Department of Public HealthTrips by planeIt’s most likely safe for children to fly this summer, as long as they’re fully masked and everyone else on the plane is, too, 86 percent of the experts said. But they said this should be done with caution — consider double masking and limiting the number and length of flights.“The risk of transmission goes up the longer the flight, but assuming everyone is masked, air travel is fairly safe.”Laura Hammitt, physician and associate professor of public health, Johns Hopkins“Until my children are vaccinated, we are not flying.”Laura Stadler, physician and professor of pediatrics, Division of Infectious Diseases, Kentucky Children’s HospitalOutdoor playgrounds and sportsAlmost two-thirds of the experts said unvaccinated children should still wear masks while at playgrounds or playing sports outdoors, even though the virus is much less likely to spread outside.“I consider masks necessary in outdoor situations when children will be very close together, which is often the case in sports and at playgrounds.”Caitlin McGrath, physician and pediatric infectious diseases fellow, University of Washington“For many sports, there is a low risk of transmission when playing outdoors unmasked, including sports such as tennis and volleyball and likely even soccer. The risk of transmission while playing unmasked goes up for contact sports.”Felice Adler, physician and associate professor of clinical pediatrics, University of California, Irvine“The only situation where I might still recommend wearing a mask is if the children are in close quarters — for example, huddled together talking on the playground or sitting together in the dugout. When they are moving around and playing, masks are not necessary.”Alison Tribble, physician and assistant professor of pediatrics, University of MichiganAdvice for vaccine-hesitant parentsThis phase of the pandemic — with children becoming more of the focus — will become easier when children under 12 can be vaccinated. But some parents are hesitant about vaccinating their children, especially considering that the risk to them from Covid-19 is still so small.Some epidemiologists and physicians were discussing this in their own families. Of the 8 percent who were unsure about vaccinating their young children, several said it was because they had not yet convinced their spouse that it was the best course of action.But as a group, the experts surveyed were unconflicted about vaccinating children. Many cited the risk of long-term physical and neurological effects of Covid-19, which are still unknown in children. And they worried about new variants of the virus that could become more dangerous for children.“We’re still learning about the long-term effects of Covid-19 in asymptomatic and mildly symptomatic previously healthy individuals,” said Ms. Ergas, of the Massachusetts Department of Public Health. “I’m not panicked about my kids getting Covid, but I’d rather they didn’t.”Others were more concerned. “I suspect that a proportion of children who have a Covid-19 infection will go on to have problems that are due to inflammation,” said Dr. Jessica Ericson, an infectious disease pediatrician at Penn State College of Medicine. “The long-term consequences of Covid-19 are unknown at this point, but unlikely to be zero. This is in contrast to vaccination, which has no plausible long-term consequences.”Beyond children’s health, they said, pediatric vaccines were necessary for the greater good. The pandemic is unlikely to end in the United States until children are vaccinated, they said. Even though children are less likely than adults to spread the coronavirus, as long as the virus can replicate, it will mutate, whether carriers are symptomatic adults or asymptomatic children. Also, even if Americans achieve widespread immunity, the virus will continue to spread and mutate in parts of the world without the same access to vaccines.“It’s a big, altruistic ask for below-12s to be vaccinated in large numbers,” said Andrew Noymer, an epidemiologist at the University of California, Irvine. “The overwhelming majority of cases are not going to be sick. It’s not for their benefit; it’s to prevent them from spreading it to others.”Dr. Andrew Handel, an infectious disease pediatrician at Stony Brook Medicine, said: “Once approved, I will enthusiastically have my children vaccinated. These vaccines are the best solution we have to the tremendous damage posed by this disease.”The costs of isolationEven as the experts urged continued caution until a pediatric vaccine arrives, they also emphasized that parents needed to weigh the risks of continued social isolation. Over all, the experts were somewhat more concerned about the mental health consequences of the pandemic for children than about its effects on their physical health.“Isolation of children is detrimental to their mental and physical health,” said Kevin Andresen, leader of the Covid response team for the Colorado Department of Public Health. “Finding safe ways to have children socialize and play needs our full attention while we continue to evaluate vaccine efficacy in this group.”Marissa Brash, chair of the department of public health at Azusa Pacific University, said: “We have done as many Zoom play dates as we can for my 9-year-old. She’s navigated Facebook friends. She’s streamed Netflix movies together over FaceTime. But nothing substitutes cartwheels and climbing trees and building sand castles.”They have started meeting a friend at a park: “The impact this has had on my daughter’s mental health is staggering.”The experts urged patience for a little longer. And many expressed optimism that children could bounce back from this difficult period.“Most children don’t mind the masks, they have hand washing down, and are much more tolerant and accepting of all these changes,” said Dr. Dirajlal-Fargo of Case Western. “Most of them have been fantastic and, if anything, have taught us how to behave during this pandemic.”Our survey was distributed by email to members of five groups: the Society for Epidemiologic Research; the Council of State and Territorial Epidemiologists; the Pediatric Infectious Diseases Society; the Decision Sciences for Child Health Collaborative; and the American Academy of Pediatrics subspecialty group on epidemiology, public health and evidence. Responses were collected between April 28 and May 10. After the announcement of the C.D.C.’s new policy on mask use for vaccinated people on May 13, we sent a series of follow-up questions to survey respondents and collected responses between Monday and Thursday. For various reasons, the number of responses differed by question.
Read more →