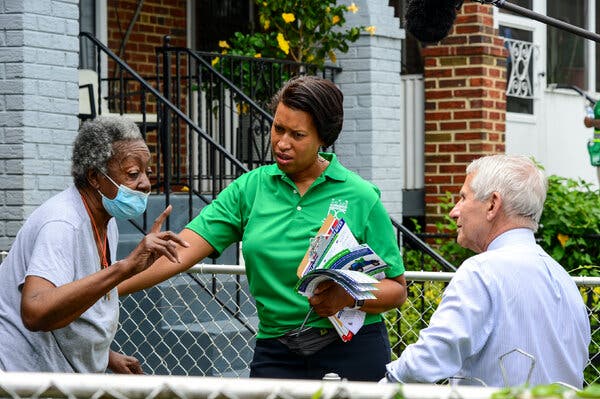With Mass Vaccination Sites Winding Down, It’s All About the ‘Ground Game’
The shift away from high-volume centers is an acknowledgment of the harder road ahead: a highly targeted push, akin to get-out-the-vote efforts, to persuade the reluctant to get shots.NEWARK — There were only six tiny vials of coronavirus vaccine in the refrigerator, one Air Force nurse on duty and a trickle of patients on Saturday morning at a federally run mass vaccination site here. A day before its doors shut for good, this once-frenetic operation was oddly quiet.The post-vaccination waiting room, with 165 socially distanced chairs, was mostly empty. The nurse, Maj. Margaret Dodd, who ordinarily cares for premature babies at Brooke Army Medical Center at Fort Sam Houston in San Antonio, had already booked her flight home. So had the pharmacist, Heather Struempf, who was headed back to nursing school in Wyoming.Across the country, one by one, mass vaccination sites are shutting down. The White House acknowledged for the first time on Tuesday that it would not reach President Biden’s goal of getting 70 percent of American adults at least partly vaccinated by July 4. The setback stems from hesitancy in certain groups, slow takeup by young adults and a swirl of other complex factors.The Newark site, which closed on Sunday, was the last of 39 federally operated mass vaccination centers that administered millions of shots over five months in 27 states. Many state-run sites are also closed or soon will be.The nation’s shift away from high-volume vaccination centers is an acknowledgment of the harder road ahead, as health officials pivot to the “ground game”: a highly targeted push, akin to a get-out-the-vote effort, to persuade the reluctant to get their shots.Mr. Biden will travel to Raleigh, N.C., on Thursday to spotlight this time-consuming work. It will not be easy — as Dr. Anthony S. Fauci, the president’s coronavirus response coordinator, discovered last weekend, when he went door-knocking in Anacostia, a majority-Black neighborhood in Washington, with Mayor Muriel E. Bowser.The Newark site once administered as many as 6,700 shots a day.Bryan Anselm for The New York TimesThe site was operated by the Federal Emergency Management Agency in conjunction with the Defense Department and other federal agencies.Bryan Anselm for The New York TimesIn an interview on Tuesday, Dr. Fauci said he and the mayor spent 90 minutes talking to people on their front porches. But even with a celebrity doctor at the door and the prospect of giveaways at the vaccination center in a high school a few blocks away, many remained hesitant. Dr. Fauci said he persuaded six to 10 people to get their shots, though he did encounter some flat refusals.“We would say, ‘OK, come on, listen: Get out, walk down the street, a couple of blocks away. We have incentives, a $51 gift certificate, you can put yourself in a raffle, you could win a year’s supplies of groceries, you could win a Jeep,’” Dr. Fauci said. “And several of them said, ‘OK, I’m on my way and I’ll go.’”But in Newark, where more than three-quarters of the population is Black or Latino, the numbers tell the story. In Essex County, N.J., which includes Newark, 70.2 percent of adults have been vaccinated. But Essex also includes wealthy suburbs; in Newark, the figure is 56 percent, Judith M. Persichilli, the state’s health commissioner, said in an interview.The Newark vaccination site, in a converted athletic facility at the New Jersey Institute of Technology that is ordinarily home to the school’s tennis teams, was set up and run by the Federal Emergency Management Agency in conjunction with the Defense Department and other federal agencies. It opened on March 31; when it was operating at full tilt, its medical staff administered as many as 6,700 shots a day.Dr. Anthony S. Fauci, right, and Mayor Muriel E. Bowser of Washington, center, went door-knocking in the city’s Anacostia neighborhood on Saturday to encourage residents to get vaccinated.Kenny Holston for The New York TimesBy Saturday, the daily tally was down to about 300. The long, corridorlike tents that had once shielded lines of patients from cold weather were empty. Of 18 registration desks, only four were in use, and most of the vaccination cubicles were unoccupied.Most of the patients, including some teenagers brought by their parents, were there for their second dose of the Pfizer-BioNTech vaccine. Many — like Abdullah Heath, 19, who took a year off after high school and will attend Rutgers University in the fall — said they were hesitant. But Rutgers requires vaccination, so Mr. Heath had little choice.“I wanted to wait to see how other people were when they took the shot,” he said.Alfredo Sahar, 36, a real estate agent originally from Argentina, said he had received his first dose on the spur of the moment, without an appointment, when he tagged along with his wife to the Newark site. The couple showed up for their second doses on Saturday with a young friend, Federico Cuadrado, 19, who was visiting from Argentina and received his first shot.“Relax this arm,” Major Dodd said as Mr. Cuadrado rolled up his sleeve. But she will not be administering his second shot; with the site now closed, he will have to go elsewhere.At the height of its vaccination drive, New Jersey had seven mass sites: six run by the state, plus the FEMA site in Newark. Two of the state sites have closed, another will shut down this week, and the last three are expected to do so in mid-July, said Ms. Persichilli, a nurse and former hospital official. She called the FEMA site, which vaccinated 221,130 people in all, “invaluable.”Maj. Margaret Dodd, right, gave Federico Cuadrado his first dose of the Pfizer-BioNTech vaccine in Newark on Saturday.Bryan Anselm for The New York TimesMr. Biden has said repeatedly that equity — making sure people of all races and incomes have the same access to care and vaccines — is crucial to his coronavirus response. FEMA determined the locations for its mass vaccination sites using the Centers for Disease Control and Prevention’s “social vulnerability index” to identify communities most in need, Deanne Criswell, the FEMA administrator, said in an interview.It was a learning experience for the agency, she said, adding that 58 percent of the roughly six million shots administered at the mass vaccination sites were given to people of color.“We didn’t have a playbook for this type of an operation,” Ms. Criswell said. (The agency now has one that is 44 pages long.)In New Jersey, traffic at the mass vaccination sites started tapering off about six weeks ago, Ms. Persichilli said. At about that time, the state moved to a “hub and spoke” strategy, creating pop-up sites in churches, barbershops and storefronts surrounding existing vaccination centers that could store and supply the vaccines.The state also has 2,000 canvassers — 1,200 paid, partly with federal taxpayer dollars, and 800 volunteers — who have knocked on 134,000 doors in areas with low vaccination rates to direct people to nearby clinics. And the Health Department is planning vaccine clinics at a rock music festival, a balloon festival and a rodeo in Atlantic City.Overall, New Jersey is way ahead of most states: 78 percent of adults have had at least one dose of a vaccine. In four states — Mississippi, Alabama, Louisiana and Wyoming — the figure is lower than 50 percent.“We’re running a marathon, and we’re in the last couple of miles, and we’re exhausted, and they’re going to be the most difficult ones,” Ms. Persichilli said. “But they are also going to be the most satisfying ones.”A photo booth outside the Newark site, which closed on Sunday.Bryan Anselm for The New York TimesThe site was the last of 39 federally operated mass vaccination centers that administered millions of shots over five months in 27 states.Bryan Anselm for The New York TimesPublic health officials know that the last mile of any vaccination campaign is indeed the hardest. The eradication of smallpox, considered the greatest public health triumph of the 20th century, came after a highly targeted global campaign that lasted two decades. Polio has still not been eradicated in some countries, Dr. Fauci said, because of vaccine hesitancy, including among women who express unfounded fears of infertility.“We should have eradicated polio a long time ago,” he said.The federal effort has been enormous, involving more than 9,000 people from across the government, as well as 30,000 National Guard members supporting Covid-19 vaccination in 58 states and territories, according to Sonya Bernstein, a senior policy adviser for the White House.With the large vaccination sites winding down, FEMA is also pivoting. The agency still supports more than 2,200 community vaccination centers and mobile vaccination units. Now FEMA is rolling out a new pilot program to offer shots at or near recovery centers that it sets up after hurricanes and other natural disasters. The first of these opened this week in St. Charles Parish, La., which has a large minority population and was devastated by Hurricane Laura last summer. Only 51 percent of the adult population in St. Charles Parish has had at least one shot, according to data from the C.D.C.Long, corridorlike tents at the Newark vaccination site once shielded lines of patients from cold weather. On Saturday, the daily tally of administered shots was down to about 300. Bryan Anselm for The New York TimesIn Newark, the mood on Saturday was bittersweet. People like Major Dodd and Ms. Struempf, thrown together in a crisis, were exchanging phone numbers with newfound friends and colleagues as they planned to go their separate ways. After living in hotels for more than two months, they were both eager to depart and wistful about the prospect.Michael Moriarty, the FEMA official who supervised the creation of the site, surveyed the scene: the vacant cubicles and chairs, the boxes of unused latex gloves, the brown paper taped to the floor to cover the tennis courts. It would not take long to undo, he said, adding, “They’ll be playing tennis here at the end of the week.”
Read more →