Strange microscopic structures found in Long COVID blood
The researchers also incorporated Artificial Intelligence tools, including machine learning, to analyze biomarker patterns. These methods allowed them to accurately differentiate Long COVID patients from healthy individuals and to pinpoint the most informative biomarker combinations. Such insights could support more precise diagnostics and future personalized treatments. small, unusual clusters of blood clotting proteins that circulate in the bloodstream. The term became widely used in 2021 after Prof Resia Pretorius of Stellenbosch University’s Department of Physiological Sciences reported finding these abnormal protein clumps in blood samples from COVID-19 patients. Their potential involvement in COVID-related clotting problems drew significant attention as the pandemic unfolded.What are neutrophil extracellular traps (NETs)?Dr. Alain Thierry and his group at the Montpellier Cancer Institute (IRCM) at INSERM in Montpellier were among the first to highlight the importance of NETs in COVID-19. NETs form when neutrophils release their DNA through a process called NETosis, creating thread-like structures filled with harmful enzymes that can quickly trap and neutralize invading microbes.Although NETs help defend against infection, producing too many of them can be harmful. Excess NET formation has been linked to serious inflammatory and clotting conditions, including severe infections, autoimmune diseases, cancer, diabetes, and arthritis. Dr. Thierry notes that ongoing overproduction of NETs, driven by cycles of inflammation and clot formation, may worsen disease severity.In light of this, the teams led by Prof Pretorius and Dr. Thierry worked together to examine whether microclots and NETs interact in patients with Long COVID.Key findingsUsing imaging flow cytometry and fluorescence microscopy, the researchers conducted detailed measurements of microclots and NETs in the plasma of individuals with Long COVID and compared the results to healthy controls. They also quantified NETs by assessing proteic markers and circulating DNA.They reported several major observations: Biomarkers linked to both microclots and NETs were significantly elevated in Long COVID patients. Patients showed not only an increased number of microclots but also larger microclots. Most notably, the team identified a structural relationship between microclots and NETs. This association appeared in all samples but was far more substantial in people with Long COVID.”This finding suggests the existence of underlying physiological interactions between microclots and NETs that, when dysregulated, may become pathogenic,” explains Dr. Thierry.
The researchers also incorporated Artificial Intelligence tools, including machine learning, to analyze biomarker patterns. These methods allowed them to accurately differentiate Long COVID patients from healthy individuals and to pinpoint the most informative biomarker combinations. Such insights could support more precise diagnostics and future personalized treatments.Prof Pretorius emphasizes that the study reveals a buildup of microclots in the plasma of Long COVID patients, likely supported by excessive NET activity: “This interaction could render microclots more resistant to fibrinolysis, promoting their persistence in circulation and contributing to chronic microvascular complications,” she explains.By clarifying how NETs may stabilize microclots, the study contributes valuable information about the biological processes involved in Long COVID. The findings also highlight potential therapeutic approaches aimed at reducing harmful clotting and inflammation.In addition, the work advances the search for new biomarkers that could help diagnose and manage Long COVID. As the authors note, “The combination of advanced imaging techniques and machine learning confers methodological robustness and contributes significantly to the ongoing scientific discourse on post-viral syndromes.”
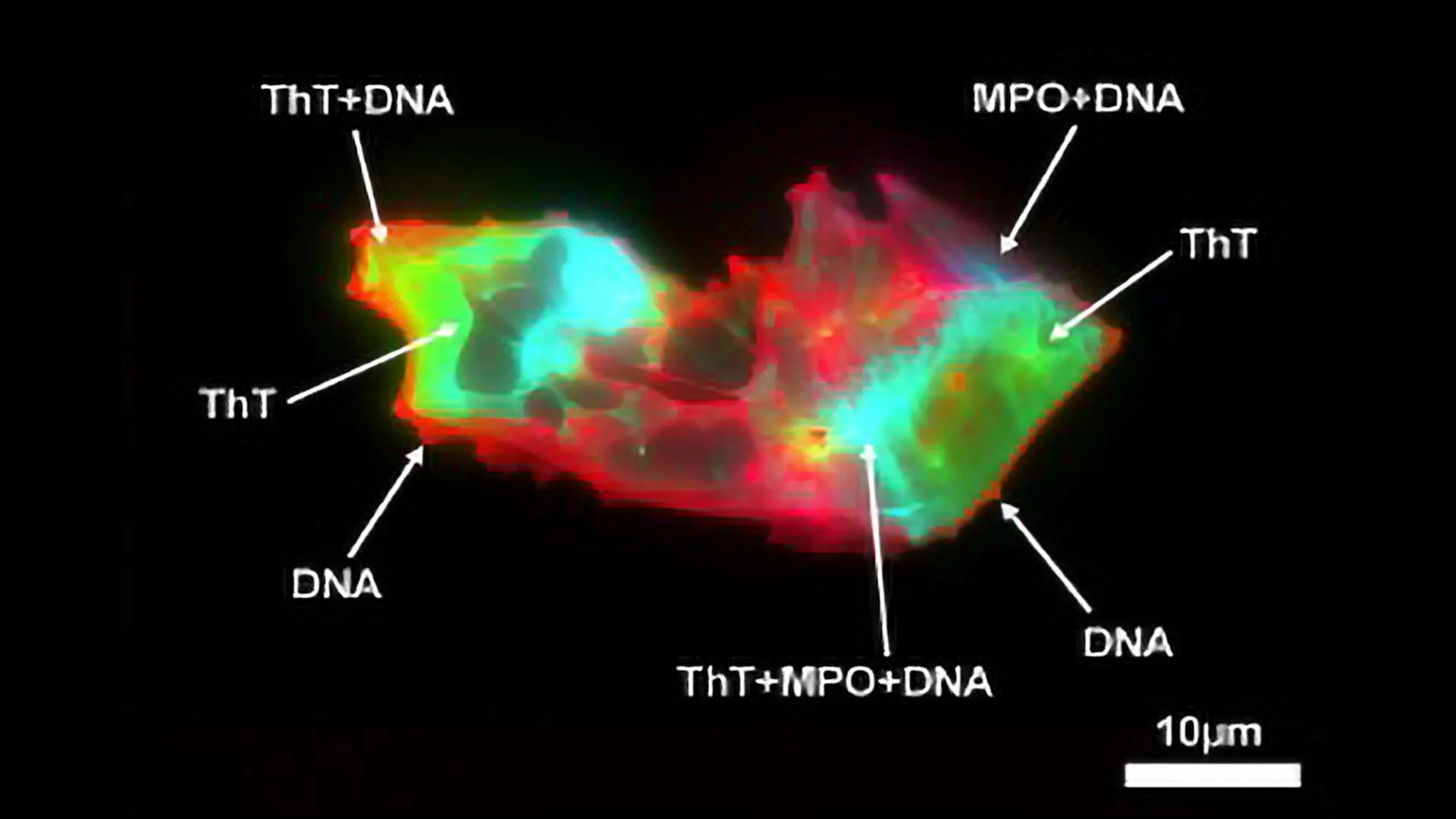
In patients with Long COVID, a new study has revealed structural association between circulating microclots and neutrophil extracellular traps (NETs).
This finding suggests the existence of underlying physiological interactions between microclots and NETS that, when dysregulated, may become pathogenic.
What are microclots?
The term microclots, recently adopted in the scientific literature, refers to abnormal clumps of blood clotting proteins circulating in a patient’s blood stream. The concept was introduced in 2021 by Prof. Resia Pretorius from Stellenbosch University’s Department of Physiological Sciences, when they found the abnormal presence of such microclots in the blood samples of COVID-19 patients. This discovery generated widespread attention during the pandemic due to its potential role in COVID-related coagulopathies.
What are neutrophil extracellular traps (NETs)?
Dr. Alain Thierry’s team at the Montpellier Cancer Institute (IRCM) at INSERM in Montpellier, was among the first to identify the critical role of NETs in the pathogenesis of COVID-19. NETs are produced through a specialised form of innate immune response known as NETosis, whereby neutrophils expel their DNA to form filamentous structures embedded with cytotoxic enzymes capable of rapidly trapping and neutralizing pathogens.
However, excessive NETs formation can become detrimental, contributing to a wide range of inflammatory and thrombotic diseases, including severe infections, autoimmune disorders, cancer, diabetes, and arthritis.
According to Dr. Thierry, it may be that persistent overproduction of NETs, fueled by self-perpetuating inflammatory and thrombotic loops, exacerbates disease severity.
In a collaborative effort, the teams of Prof. Pretorius and Dr. Thierry investigated the potential interaction between microclots and NETs in the context of Long COVID.
Key findings
Using imaging flow cytometry and fluorescence microscopy, they performed a quantitative and structural analysis of microclots and NETs in the plasma of Long COVID patients, compared to healthy controls. NETs were also quantified by analyzing NETs proteic markers and circulating DNA. They observed a significant increase in biomarkers associated with both microclots and NETs in patient samples. Microclots were not only more abundant but also larger in size among patients. Most importantly, they discovered a previously unreported structural association between microclots and NETs, observed in all subjects but markedly more pronounced in Long COVID patients.”This finding suggests the existence of underlying physiological interactions between microclots and NETs that, when dysregulated, may become pathogenic,” explains Dr. Thierry.
Furthermore, the integration of Artificial Intelligence tools, such as machine learning, into the biomarker analysis enabled them to distinguish Long COVID patients from healthy individuals with high accuracy. The algorithms identified the most predictive biomarker combinations, enhancing diagnostic reliability and paving the way for personalized medicine approaches.
According to Prof. Pretorius, the results reveal a significant accumulation of microclots in the plasma of Long COVID patients, likely driven and stabilized by excessive NETs production: “This interaction could render microclots more resistant to fibrinolysis, promoting their persistence in circulation and contributing to chronic microvascular complications,” she explains.
By identifying the mechanistic role of NETs in microclot stabilization, this study provides new insight into the pathophysiology of Long COVID. These findings support the development of targeted therapeutic strategies aimed at modulating thrombo-inflammatory responses.
Finally, the study paves the way for the development of novel biomarkers for diagnosis and management: “The combination of advanced imaging techniques and machine learning confers methodological robustness and contributes significantly to the ongoing scientific discourse on post-viral syndromes,” they conclude.